Share On Social!
Hospital closures have become the norm in many rural areas.
Now, rural pharmacies are headed on the same path, according to a U.S. News Report.
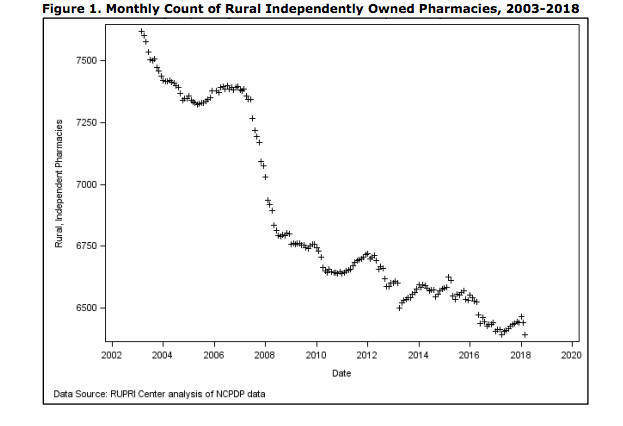
Over the past 16 years, 1,231 rural, independently-owned pharmacies have closed. That’s 16% of all rural pharmacies.
Fewer than 6,400 pharmacies are left in rural communities.
Rural communities that had at least one retail (independent, chain, or franchise) pharmacy in March 2003 had no retail pharmacy in March 2018, according to RUPRI Center for Rural Health Policy Analysis Rural Policy Brief.
Residents of rural communities now have to travel great distances for medications and/or turn to mail-order prescriptions that make it impossible for in-person consultation concerning questions about the medication.
“Closure of pharmacies in rural communities can have grave implications for the population’s access to health services, requiring them to travel to another community for pharmacy services or to rely on mail order services that cannot provide clinical services,” states the policy brief.
What’s Causing The Closures?
The implementation of Medicare Part D attributes to many financial challenges that rural pharmacies face. Medicare Part D has lower reimbursement rates when compared to actual costs and previous out-of-pocket payments.
“The biggest spike in rural pharmacy closures occurred a few years ago, after the full implementation of Medicare Part D,” Keith Mueller, director of the RUPRI Center, which is based at the University of Iowa and supported by the Federal Office of Rural Health Policy, told U.S. News.
Another reason: competing chain companies like CVS and Walgreens.
“They’re the kinds of issues that if you’re at the scale of a CVS, it’s not the dealbreaker,” Mueller said. “But it is for a local independent pharmacy.”
How Closures Affect Overall Health
Access to a pharmacy plays a vital role in patient safety and overall health. Convenience and location affects whether people take their prescription drugs as recommended.

“If you have to drive 60 miles to pick up your drug, you’re not going to get your refills on time as often as you should,” Bree Watzak, a clinical associate professor of pharmacy practice in the College of Pharmacy and the Rural and Community Health Institute at Texas A&M University, told U.S. News. “Whereas, if it’s right there where you live, that makes it easier for you to take the medications that you need.”
Local pharmacies also serve as telehealth sites. Patients can check their vitals, use the blood pressure machine, and check their blood glucose. This information can be facilitated by the pharmacist and transmitted to the physician on screen.
Solutions To Combat Rural Pharmacy Closures
There are numerous ways for rural community members to get involved to improve the presence of pharmacists and pharmacies, according to the Center For Rural Policy and Development.
- Risk for loss of local, rural pharmacy services. Rural residents need to engage and understand the issues as to why pharmacies are closing.
- Advocate. Speak up with state and federal legislators on issues, like low reimbursement rates, that affect medication use and accessibility.
- Physician education. Students originally from rural areas and residents trained in rural areas are more likely to practice in rural areas.
- Understanding the role of a pharmacy. It is more than the basic access point for medications. As mentioned previously, they provide basic, preventive screenings as well.
“Communities and health care leaders should seek to partner with pharmacists to develop mechanisms that integrate pharmacists more fully into the rural community’s health care system,” according to the Center For Rural Policy and Development.
“Pharmacists contribute in many ways to creating successful outcomes of medication therapy. The presence of pharmacy services in a local community is a key component of the broader health care delivery system, as well as the strength of the local economy.”
Editor’s Note: Photo of the closing of a Walgreen’s is from the Anniston Star.
Explore More:
Healthcare AccessBy The Numbers
142
Percent
Expected rise in Latino cancer cases in coming years