
Share On Social!
No money. No quality childcare. No social or legal support.
These big stressors plague many parents, and can spur domestic violence and child maltreatment, hampering a child’s early and future development.
Fortunately, Project DULCE is testing a unique solution.
DULCE adds a “family specialist” to a child’s pediatric healthcare team. The Family Specialist builds relationships of trust and respect with enrolled families and connects families to social services if they want ─ like food stamps, housing vouchers, and legal services ─ to reduce economic stress and prevent maltreatment.
Public health advocates often talk about health and quality of life in an “upstream-downstream” fashion. They want to highlight the importance of prevention and the influence of social, economic, environmental and cultural factors on health.
A downstream focus might be individual-level education or intervention to address child maltreatment.
A more upstream strategy is to address economic hardship, which can then prevent the maltreatment.
A Big Upstream Factor: Economic Hardship
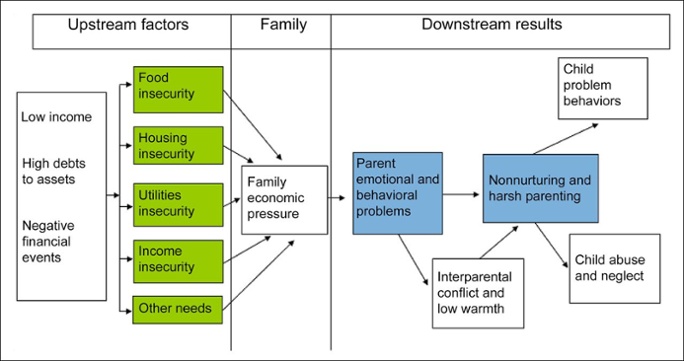
Many Latino children are born into economic hardship. They face insecurity around food, housing, utilities, income and other resources. A lack of economic and social support for parents puts big economic pressure on these families, according to a Salud America! research review.
These conditions indirectly lead to child abuse and neglect.
The estimated lifetime financial costs associated with one year of child maltreatment in the U.S. is about $124 billion, according to the Centers for Disease Control and Prevention (CDC).
“No child should ever be the victim of abuse or neglect – nor do they have to be,” said Linda C. Degutis of the CDC′s National Center for Injury Prevention and Control in a 2012 press release. “The human and financial costs can be prevented through prevention of child maltreatment.”
There are ways to address upstream economic hardship.
Early provision of concrete supports, like adult education and job training, food stamps, utility service, and housing subsidies, may reduce parental stress and protect against child maltreatment.
Legal services also can help.
“Civil rights laws and public interest laws are levers for health equity,” said Samantha Morton, CEO of MLPB (formerly known as Medical-Legal Partnership | Boston).
Studies show that when legal services and expertise are integrated into healthcare settings to address social needs, people are admitted to the hospital less frequently, more likely to take their medications as prescribed, and report lower levels of stress, according to Project DULCE website.
Project DULCE: Targeting the Upstream
Enter, Project DULCE.
 To improve care of newborns and their families, researchers with Boston Medical Center’s Pediatrics Department partnered with MLPB and others to pilot Project DULCE (Developmental Understanding and Legal Collaboration for Everyone).
To improve care of newborns and their families, researchers with Boston Medical Center’s Pediatrics Department partnered with MLPB and others to pilot Project DULCE (Developmental Understanding and Legal Collaboration for Everyone).
This medical-plus-legal initiative recruited families with kids from birth to age 6 months of age from an urban hospital from 2010-2012. More than 90% of participants were Latino or other minorities.
The project randomly assigned families to a DULCE “Family Specialist” with knowledge and ongoing training in child development milestones and in concrete support problem-solving, backed by legal partners at MLPB. The control group received standard of care and, if they wanted, an unrelated infant safety program. The intervention used the Strengthening Families Protective Factors Framework and parts of the Medical-Legal Partnerships approach.
The 6-month intervention provided:
- collaborative routine visits with the family, the pediatrician, and the family specialist;
- structured screening and family-driven problem-solving re: barriers to concrete supports;
- a weekly case review meeting attended by all members of the interdisciplinary DULCE team;
- home visits by the family specialist as desired; and
- Ongoing access to the family specialist by telephone, e-mail, text, or in person.
The results were astounding.
Total number of emergency department visits was significantly lower in the DULCE group than in the control group at 6 months. DULCE accelerated access to concrete supports for newborns and their families, according to a July 2015 study in Pediatrics.
Scaling Up the Upstream Effect of DULCE
In late 2015, with funding from the JPB Foundation, the Center for the Study of Social Policy (CSSP) launched a three-year national demonstration project to refine and scale DULCE in five counties in California, Florida and Vermont. MLPB is part of the national technical assistance team supporting new DULCE communities.
Health centers in these five counties integrated a Family Specialist within their Pediatric practices, alongside structured integration of public interest law advocates and embrace of the Brazelton Touchpoints approach.

Similar to community health workers, some DULCE family specialists themselves have lived experience as an immigrant in this country, navigating complex bureaucracies, systems, policies, and programs personally and professionally.
“There isn’t just one immigrant experience,” Morton said, but in DULCE communities with high immigrant populations, even some level of shared lived immigrant experience can be critical to effectively developing trust with families.
Family specialists take medical care beyond the medical home and connect families to appropriate economic, social, and legal services and resources, like housing assistance. They meet families at the infant’s routine healthcare visits as well as offer home visits and telephone, email and text-messaging support.
“The cohort of DULCE Family Specialists is really gifted at bringing trauma-informed and strengths-based lenses to their work so that enrolled families are more likely to receive and use knowledge to make informed decisions about applying for public benefits, addressing poor housing conditions, or seeking protection from domestic violence,” Morton said.
DULCE proactively addresses social determinants of health and mitigates the risk factors for early life stress through the combined efforts of pediatric, legal, and early childhood providers.
The importance of providing legal services was emphasized for DULCE teams after the dramatic tidal wave of law, policy and regulatory change related to federal immigration policy in early 2017, Morton said.
“The interesting thing about DULCE is the addition of non-traditional tools to both the early childhood and health equity toolboxes,” Morton said.
In 2017, the Rand Corporation found a reduction in use of public services and emergency medical services by participants in the successful Housing for Health initiative in Los Angeles.
“Communities need housing solutions for people across the age and health continuum-before the children grow up to be high-need, high-cost adults,” said Morton in Nonprofit Quarterly on the heels of this report.
It makes sense for healthcare to account for families’ social and economic needs, like housing, when assessing their care needs and developing care plans with them.
Learn more about Project DULCE.
Spread the word about how healthcare organizations are implementing upstream strategies to reduce family economic stress, prevent child maltreatment and boost early childhood development!
By The Numbers
28
percent
of Latino kids suffer four or more adverse childhood experiences (ACES).



