Share On Social!
This is part of the “Advancing the Science of Cancer in Latinos: 2022 Conference Proceedings,” which summarizes findings and discussions of the 2022 Advancing the Science of Cancer in Latinos Conference on Feb. 23-25, 2022, in San Antonio, Texas.
Cancer Screening in Puerto Rico Challenges and Opportunities to Address Health Disparities
Dr. Guillermo Tortolero-Luna is Director of the Division of Cancer Control and Population Sciences Program at the University of Puerto Rico Comprehensive Cancer Center.
Cancer statistics in Puerto Rico

Dr. Tortolero-Luna began by describing the cancer landscape in Puerto Rico. In 2012, malignant cancers became the cause of death with the highest age-adjusted mortality rate in the territory. The highest cancer sites among Puerto Rican men are prostate, colon/rectum, and lung/bronchus; while cancer in women most often affects the breast, followed by colon/rectum. The same cancer sites also have the highest mortality in men and women, with the top three sites in men causing 42.6% of all cancer deaths, and the top two sites in women causing 32.2% of cancer deaths.
Although incidence rates of prostate and colon/rectum cancer in Puerto Rican men have remained constant since 2000, lung/bronchus cancer is decreasing. In women, although incidence rates for colon/rectum cancer have remained constant since 2000, breast cancer rates are increasing. Mortality trends in men have, as expected, decreased over the past two decades, with the exception being the unchanged mortality rate of colon/rectum cancer. In women, mortality rates for colon/rectum cancer have improved, but breast cancer mortality rates have remained constant.
Cancer screening in Puerto Rico
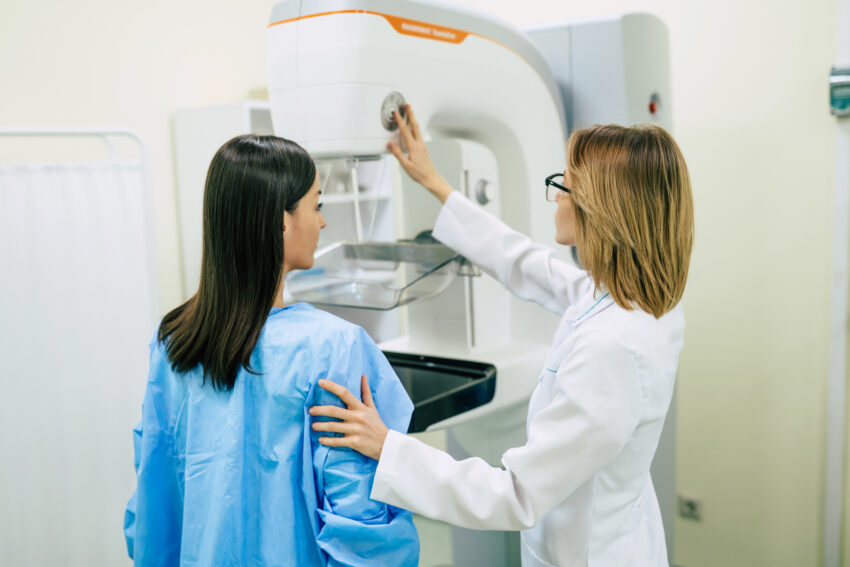
Cancer screening rates in Puerto Rico in 2020 were slightly lower than in the US. In Puerto Rico, 73.3% of people aged 50 to 75 had been recently screened for colorectal cancer, compared with 74.3% of the general US population. Furthermore, 70.4% of Puerto Rican women over the age of 40 had received a mammogram in the last two years, compared with 71.5% of US women.
Many barriers are responsible for this disparity in breast cancer screening: religious beliefs, embarrassment, pain with procedure, worry about work, being a caregiver for another, couples issues, fear of diagnosis, physical or mental impairment, economic issues, transportation, and concern about COVID-19. Barriers for colorectal screening are similar, with the added burdens of fear of the test, lack of knowledge about the disease, concern about insurance coverage, and lack of physician recommendation.
The PRBCCEDP
The Puerto Rico Breast and Cervical Cancer Prevention and Early Detection Program (PRBCCEDP) has been working to combat these trends since 2017. By increasing population-based approaches and working within health system clinics and communities, the PRBCCEDP has focused on decreasing disparities in screening through evidence-based interventions (EBIs). The program has sought to address barriers to screening by using a multifaceted approach that includes workplace approaches, external partnerships, health system interventions, community-clinical linkages, and cancer data and surveillance.
Future plans of the PRBCCEDP include using surveillance systems and population-based surveys to assess cancer burden, examining health disparities, focusing program efforts, and addressing social determinants of health (SDOH). The PRBCCEDP will also support partnerships for cancer control and prevention as well as deliver cancer screening to primary care clinics that serve women impacted by health inequities.
Disparities and solutions
Demographics and socioeconomic factors in Puerto Rico are very different than in the US. Residents over the age of 65 make up 21.3% of the Puerto Rican population, for example, compared with 16.6% of the US population. Only 78.8% of Puerto Rican residents have a high school education or higher, compared with 88.6% of US residents. Even more startling, the Puerto Rican median household income is $20,474, compared to $65,712 in the US. These disparities are partially due to recent economic crises, natural disasters, low birth rates, and the emigration of young Puerto Rican men and women to the US, resulting in an 11.8% decrease in population since 2010.
Partially because of these socioeconomic disparities, addressing cancer health disparities in Puerto Rico is a multifaceted problem. One important step towards a solution is the use of burden data to identify and describe populations experiencing the greatest disparities and the subsequent allocation of resources to prioritize these populations. Once populations have been identified, it is important to find partners with experience working within that population and expertise in addressing under-resourced communities. Engaging communities to help identify root causes and solutions, and identifying community resources is also key. Finally, efforts must be made to evaluate outreach efforts, monitor progress, and measure impact on reducing disparities.
Dr. Tortolero-Luna closed by discussing how partnerships in cancer control in Puerto Rico, organized by the Coalición para el Control de Cáncer en Puerto Rico, are focused on these very solutions. Along with the PRBCCEDP, many other organizations participate in this effort, including Registro Central de Cáncer de Puerto Rico, immunization programs, tobacco control programs, academic and medical institutions, and many more. Through collaboration and partnership, cancer control in Puerto Rico can make substantial and measurable steps toward a more equitable future.
Practice Transformation to Improve Cancer Screening Outcomes at an Academic Medical Center
Dr. Rebecca Jones is Faculty Associate at the Institute for Health Promotion Research at UT Health San Antonio (UTHSA).
VBC and DSRIP

Dr. Jones began by describing Value-Based Care (VBC) Programs, which reward health care providers with incentive payments for the quality of care they provide to their patients. This model has four key aims: improving the patient experience of care, improving the health of individuals and populations, reducing the cost of healthcare, and improving the work life of health professionals.
Dr. Jones presented another type of program as well, the Delivery System Reform Incentive Payment (DSRIP) program, which focuses on four key areas: infrastructure development, system redesign, clinical outcome improvements, and population-focused improvements. In 2011, Texas received federal approval for the 1115 Healthcare Transformation Waiver, which supported the DSRIP program pool, incentivizing the transformation of service delivery practices to improve quality, health status, patient experience, coordination, and cost-effectiveness. In 2017, the Texas DSRIP Program included cancer screening performance as a quality metric.
Practice transformation in Texas
Based on knowledge of these two programs, Dr. Jones and her colleagues at UTHSA began a practice transformation initiative aimed at improving cancer screening rates among Medicaid, low-income, and uninsured patient populations. Major findings from a root cause analysis conducted in 2017 were as follows: cancer screening, ordering, and scheduling were variable across primary care clinics; barriers to ordering screenings included not having information on patient’s previous screenings; and health IT, the quality department, and primary care were central departments in improving performance.
Three key departments
The health IT department was responsible for data maintenance, data optimization, data reporting, and aligning electronic health record workflows. To improve performance cancer screening rates, this department developed registry dashboards to assist in identifying patients in need of a cancer screening; developed flags in patients’ medical records to display needed screenings; optimized forms to standardize the capture of screening history; optimized order forms; and created result notification reminders.
In Dr. Jones’s initiative, quality departments were responsible for overseeing and supporting UTHSA-managed care contracts, such as the DSRIP Program. This meant that the quality department interacted in real time with primary care clinics to remind clinics of patients with upcoming appointments and screening needs. The quality department also communicated with patients to retrieve cancer screening records and/or schedule screenings, and made data-driven decisions based on recommendations from a team of data analysts.
The final department recommendation involved a VBC taskforce and the primary care department. The task force convened twice a month to discuss performance and intersecting roles between health IT, primary care, and the quality department. Major focuses were educating clinicians and clinic staff on cancer screening guidelines; communicating preferred clinic workflows to health IT and the quality department; and approving protocols and scripts to be used by the quality department when reaching out to patients. Medical directors, clinic managers, quality department leaders, and patient experience members served on the task force, giving a diversity of perspective. Based on recommendations by the task force, primary care clinics were responsible for reviewing registry dashboards daily, capturing screening history, ordering cancer screenings, and communicating cancer screening results.
Initial successes and goals for the future
Dr. Jones closed her presentation by outlining the successes of the program, as well as directions for future growth. The practice transformation program initiated by UTHSA, and spurred by the Texas DSRIP program, seemed to have a positive impact on cancer screening. From 2017 to 2018, colorectal cancer screening prevalence increased by 85% (PR: 1.85, 95%CI: 1.63-2.11); cervical cancer screening prevalence increased by 44% (PR: 1.44, 95%CI: 1.18-1.76); however, increase in breast cancer screening prevalence did not reach statistical significance (PR: 1.11, 95%CI: 0.98-1.27). The quality department, primarily focused on retrieving records and scheduling, achieved these increases in cancer screenings through health IT empowerment, record retrieval, and in-clinic intervention; but more work is needed to make these changes sustainable. Effective workflows and health IT enhancements are key in the push to scale screening efforts to other care contracts. Importantly, partnerships with VBC programs represent an incredible growth opportunity for researchers and organizations that have successful cancer screening initiatives.
Despite early successes, more work is needed. One avenue for further change, and a future focus of the program, is the involvement of community health workers (CHWs). CHWs can provide cancer screening education, screen for social determinants of health and address barriers, schedule screenings, and follow patients until screenings are complete. By using CHWs, as well as the established program of practice transformation, Dr. Jones and colleagues hope to make meaningful strides in cancer screening rates throughout the state of Texas.
Explore More:
CancerBy The Numbers
142
Percent
Expected rise in Latino cancer cases in coming years



