Share On Social!
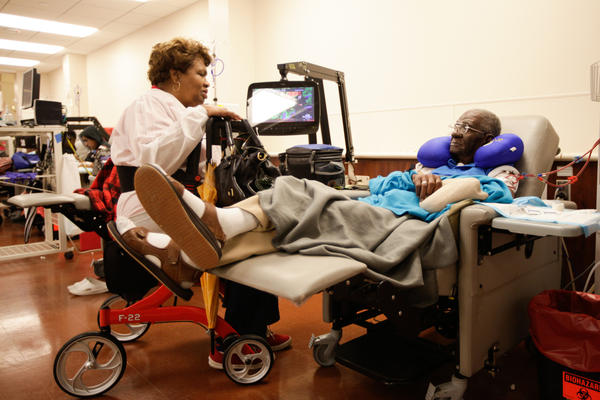
Chronic kidney disease is a crisis in the U.S. — yet, the intersection of transportation and healthcare is failing.
Public transportation agencies, healthcare providers, and patients are concerned about the rising demand, cost of providing dialysis trips for patients with the illness.
Of the forms of dialysis transportation, ambulance rides only make up 5% of trips in the US. However, they account for half of the $3 billion spent annually on dialysis transportation, according to a 2013 study in the Journal of Health Economics and Outcomes Research.
Costs could be reduced by one-third if ambulance use dropped to 1% of trips.
Gathering Needed Data
Before policy could change, all parties involved needed to know the lay of the land.
In 2016, researchers with Cooperative Research Programs of the Transportation Research Board conducted surveys of transit agencies, dialysis facilities, and dialysis patients.
Then they collected information and data from healthcare professionals on the research team to develop a forecasting tool, which estimates the needs, costs for dialysis transportation.
The data tool provides estimates of:
- Current and projected demand for public sector trips to kidney dialysis facilities
- Current and projected cost of this transportation
- Potential decreases in demand for, and cost of, public sector trips if use of home dialysis increases beyond current rates (“what if” scenarios)
Three years later, the team released their pre-publication report, “Dialysis Transportation: Intersection of Transportation and Healthcare.”
The report explores:
- Chronic kidney disease
- The challenges of dialysis transportation and transportation funding,
- Demand and costs for dialysis transportation
- Initiatives in both the healthcare and transportation organizations
“Without reliable and timely transportation, patients with chronic diseases may miss or delay appointments, which may lead to poorer management of the disease and thus poorer health outcomes,” the report states.
Transportation is a necessary partner for ongoing healthcare.
Increasing Demand for Dialysis Transportation
Approximately 30 million U.S. adults have chronic kidney disease.
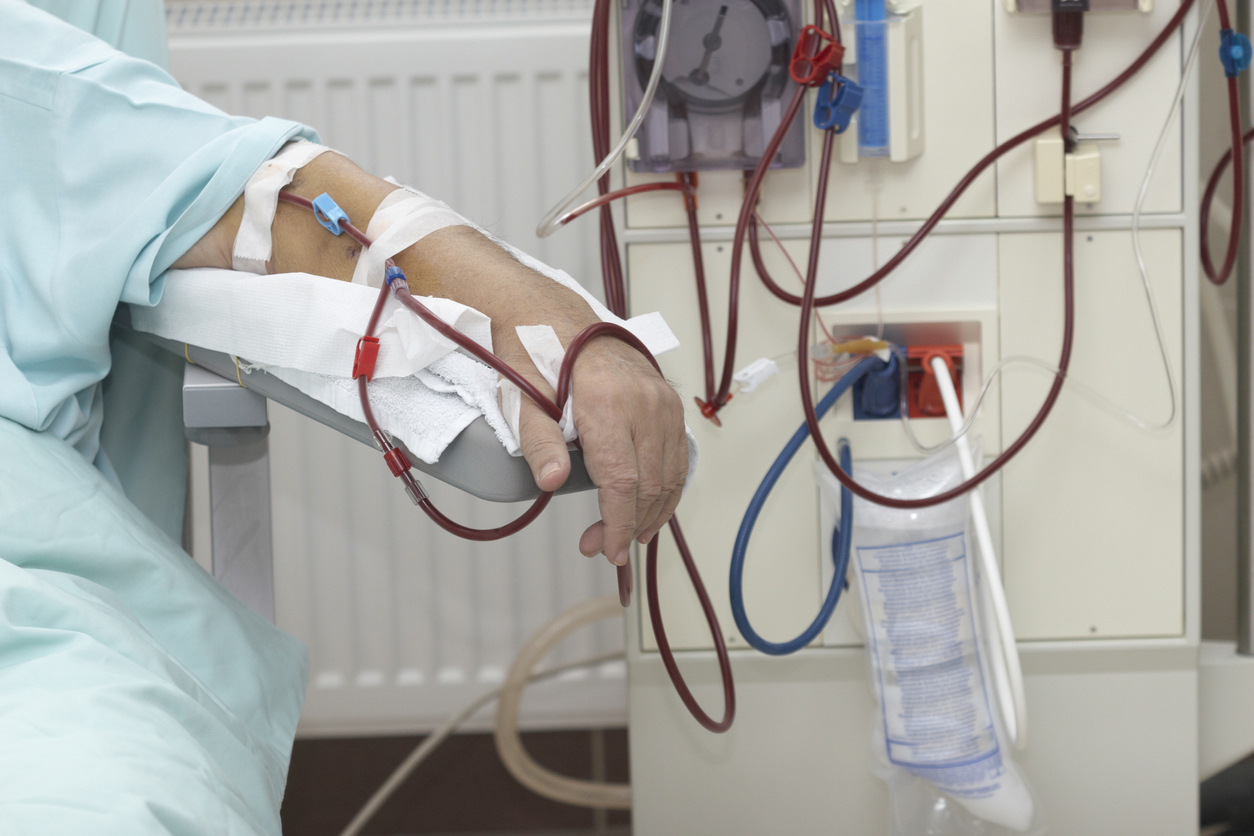
Worse, an increasing number of those will likely progress to the disease’s fifth and final stage when the kidneys fail, or end stage renal disease, according to the report.
From 2000 to 2015, the number of prevalent end stage renal disease patients increased by 80%.
Diabetes is the most common cause of end stage renal disease.
Latinos are almost twice as likely to have diabetes as white Americans, and 1.5 times more likely to have kidney failure when compared to other Americans, according to the Kidney Foundation.
In 2015, nearly 500,000 patients were receiving kidney dialysis for end stage renal disease.
Dialysis is required three days each week, meaning patients need transportation to and from their dialysis facility three times per week, translating to almost 139 million one-way trips annually for dialysis.
However, only 26% of patients drive themselves, and 20% are driven by family or friends, according to the report.
Approximately half of patients rely on public sector transportation modes—ADA paratransit, Medicaid’s non-emergency medical transportation, Veterans Administration (VA) vehicles, human service agencies, taxis, and ambulances.
The annual cost for one patient is $8,900.
Using data from this research project, researchers estimate that public sector trips to dialysis facilities costs almost $2 billion annually.
This trend will only grow.
Challenges
Unreliability is the primary problem, and it affects, patients, providers, transit agencies, and other transit riders.
Roughly 875 of nephrology social workers reported that transportation issues negatively impact patients’ dialysis treatment.
Patients and social workers also report that when transportation is unreliable, it results in patients’ stress, anxiety, and missed or shortened dialysis treatment. This can cascade into negative health outcomes and increased hospitalizations.
Healthcare providers and social workers spend hours dealing with delays, cancellations, and no-shows — costing providers and patients.
 Even patients with private transportation are concerned about the unreliability of public transportation. They understand the overarching problem: If they cannot drive themselves, they too will be dependent on the public sector.
Even patients with private transportation are concerned about the unreliability of public transportation. They understand the overarching problem: If they cannot drive themselves, they too will be dependent on the public sector.
Transit agencies are alarmed about the increasing number of trips dedicated for dialysis as well as patient and social workers’ lack of understanding about public transit’ constraints.
Nearly half of urban transit agencies and one-third of rural transit agencies reported that dialysis trips make up 10% or more of all specialized trips, according to the report.
Dialysis patients need trip flexibility; however, due to the legal framework of ADA paratransit, agencies are prohibited from prioritizing a trip’s purpose. If a patient is delayed, agencies are forced to re-route vehicles and return for that patient at a later time or find another vehicle with availability.
Transit agencies also report scheduling complications due to dialysis facility delays or changes. It was also noted that some dialysis facilities are not cooperative, resulting in less efficient and more costly transportation service.
Due to patients’ different treatment times and dispersed trip origins, limited grouping of dialysis trips lowered the productivity of transit agencies
Using the data tool, researchers estimated cost per specialized trip in four different sizes of community:
- $35.01 for large metro area transit agencies;
- $32.19 for large city agencies;
- $29.58 for smaller city agencies; and
- $26.22 for transit agencies in rural areas and small communities.
Yet, public transportation agencies receive no special funding for dialysis trips.
Although, Medicare does pay for ambulance service, an extremely costly alternative, it does not compensate for routine dialysis transportation.
Medicaid patients, however, receive free transportation. Still, social workers report it is not reliable and transportation is not always provided if Medicaid is the patient’s secondary insurance.
Additionally, the shifting of Medicaid non-emergency trips to public transit agencies’ ADA paratransit without coordination with Medicaid on funding is a concern for public transit.
“There is ‘hesitation among state Medicaid directors’ to pursue coordination with public transit since it “has not been a typical partnership in the past,” according to the report.
What Can Be Done?
The report provides various initiatives from both the healthcare and transportation perspectives to address the growing need for dialysis transportation.
Healthcare initiatives:
Healthcare providers, dialysis facilities funding and providing transportation:
Federally qualified health centers can use Health Resources and Service Administration (HRSA) grants to fund transportation as an enabling service
 The Program of All-Inclusive Care for the Elderly (PACE) program receives payments from Medicaid or Medicare for supportive services, such as transportation. PACE programs provide, on average, 16 monthly trips per participant.
The Program of All-Inclusive Care for the Elderly (PACE) program receives payments from Medicaid or Medicare for supportive services, such as transportation. PACE programs provide, on average, 16 monthly trips per participant.
Additionally, healthcare providers have varying arrangements with transportation network companies. Denver Health Medical Center, for example, provides patients with alternative transportation options. The first months of their collaboration with Lyft provided more than 200 rides at an average cost of $7.40 per ride.
Medicaid backing social interventions:
Communities should work toward improving coordination and cost-sharing with their state’s Medicaid agency for dialysis trips. State plan amendments can specify certain types of services to be paid by Medicaid. They can also specifically mention transportation services as one of the case management-related covered services. Waivers could allow for inclusion of social services, like transportation, beyond what traditional Medicaid requires.
Increase the use of home dialysis:
After the training period for home dialysis, some patients only need two to six one-way trips per month for dialysis-related appointments. However, others could need up to 24 monthly one-way trips. Home dialysis would not only reduce the need for dialysis transportation, but it may also improve patient independence and quality of life.
Address diabetes:
Healthcare programs can reduce the incidence of end stage renal disease through diabetes prevention and management programs.
The Special Diabetes Program for Indians (SDPI) has allocated $150 million annually since 1997 for community-level programs to avert and treat diabetes among Native Americans. End stage renal disease for Native Americans decreased 43% from 2000 to 2011, a greater rate than any other racial group in the country.
“Transportation is literally a primary means for improving access to care, and one might surmise that increased support and resources for transportation to dialysis would enhance the access to care strategy and further reduce total hospitalizations and readmissions,” the report states. “This would lead to not only lower Medicare spending but also healthcare improvements for dialysis patients.”
Transit initiatives:
Transit policies that provide efficient rider service:
Camden County, New Jersey’s (18.1 % Latino) transit agency adopted a fare policy that encourages dialysis riders to have treatment at the facility closest to their trip origin. Currently, all the dialysis riders served by that agency use the center closest to their home. Adoption of the policy initiated cooperation and coordination between the transit agency and dialysis centers.
The transit agency in Olympia, Washington (7.4 % Latino) set up a subscription service to automatically schedule routine trips for riders.
Education and outreach to dialysis facilities and transit riders:
San Bernardino Valley (64.3% Latino), California’s transit agency created a ten-minute presentation, “ADA Paratransit 101,” for social workers and other staff at dialysis centers. It covered what their agency can and cannot do for riders with disabilities, per mandated federal requirements.
Ride Connection, a Portland, Oregon (9.7% Latino) based non-profit, developed a training course for transportation operating staff about end stage renal disease and the effects of dialysis on patients. The group also trained dialysis clinic social workers about the complexities of trip scheduling and transit operations.
The Jacksonville Transportation Authority holds regular meetings with all 38 local dialysis centers to explain paratransit services, service changes, and to discuss challenges from the dialysis center’s perspective.
Operational strategies deployed to serve dialysis riders more effectively:

The Phoenix Dialysis Transportation Program offers dialysis patients voucher subsidies for 75% of the cost of a taxi trip with one of 14 participating taxi companies. The initiative served 75 dialysis riders in 2017, providing over 17,300 trips at half the cost of the ADA paratransit service.
Flint, Michigan’s (3.9% Latino) Mass Transportation Authority uses its mobility management function to coordinate trip scheduling for the dialysis riders directly with the 14 dialysis facilities in the service area.
Facilitating Access to Coordinated Transportation, a non-profit in Oceanside, California (35.1% Latino), organized a brokerage to purchase trips in bulk and at reduced rates from private and non-profit providers. The group then works directly with dialysis riders to schedules trips. In 2017, the group provided over 2,900 trips for dialysis.
Ride Connection, a non-profit in Portland, Oregon (9.7% Latino) piloted a three-prong program with both urban and rural dialysis clinics. The pilot called for one dispatcher to handle all calls for dialysis trips; established a more flexible wait time for return trips; and stopped grouping trips for return trips.
Coordination with dialysis facilities to plan and schedule trips for dialysis riders:
County transit staff, in Washington County, Maryland (5% Latino), developed relationships with the dialysis centers and nursing homes to coordinate patient treatment times, leading to more shared riding. One center even has a staffer assigned to coordinated transportation.
Ride Connection, a non-profit in Portland, Oregon worked with a dialysis clinic in an urban setting and in a rural area to better align trip schedules and dialysis treatments times in consideration of the geographic location of patients’ trip origin. Transit agencies may find it worthwhile to approach the dialysis clinics they serve with an offer to work with clinic staff to coordinate transportation and treatment.
Funding beyond tradition public transit grants:
The transportation authority in Idaho Falls, Idaho (14.6% Latino) received funding from the Kidney Foundation, which purchases passes for selected dialysis patients.
Through a public-private partnership in Baltimore County, Maryland (5.5% Latino), a demand response public transit system received financial support directly from hospitals and medical facilities.
Kennebec Valley Community Action Program, a non-profit in Waterville, Maine (2.4% Latino) received funding from the United Way to support dialysis transportation. Transit agencies can now approach medical facilities that they serve through their day-to-day operation and seek funding support.
Both healthcare providers and public transportation agencies play a significant role in providing and funding millions of trips for dialysis every year.
Share this with healthcare providers and public transportation agencies in your community. See if you can start or support action to improve access to affordable, reliable, and timely dialysis transportation.
By The Numbers
27
percent
of Latinos rely on public transit (compared to 14% of whites).



