Share On Social!
Forty years after the virus was discovered, an HIV vaccine is finally in development.
Moderna and the International AIDS Vaccine Initiative (IAVI) are launching the first clinical trial for an HIV vaccine.
“The search for an HIV vaccine has been long and challenging, and having new tools in terms of immunogens and platforms could be the key to making rapid progress toward an urgently needed, effective HIV vaccine,” said Mark Feinberg, president and CEO of IAVI, according to a press release.
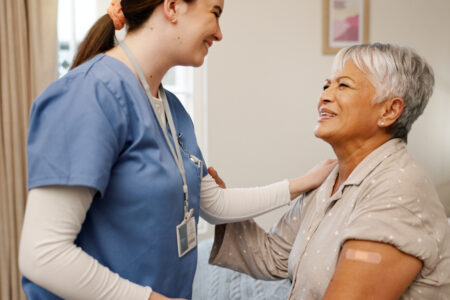
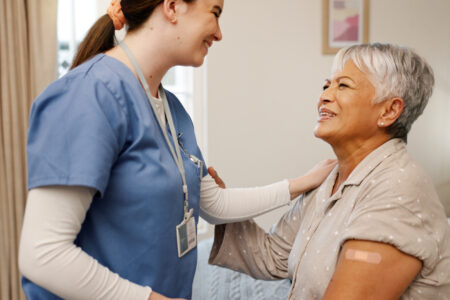
This vaccine is particularly impactful for Latinos and other people of color, who are disproportionately affected by HIV and AIDS and are underrepresented in clinical trials.
Learn more about the HIV vaccine clinical trial, how Latinos are impacted by HIV/AIDS, and how clinical trials can help stop HIV.
The First HIV Vaccine
The HIV vaccine is being developed by Moderna and IAVI, with support from the Bill and Melinda Gates Foundation.
The vaccine uses the same mRNA technology as the COVID-19 vaccines.
“The coronavirus pandemic has marshaled global resources, and billions of dollars from governments and private companies, into research into coronavirus vaccines, which were fast-tracked and developed in record time,” according to the Washington Post.
Researchers believe the new technology using mRNA particles will be more successful than previous failed versions of an HIV vaccine.
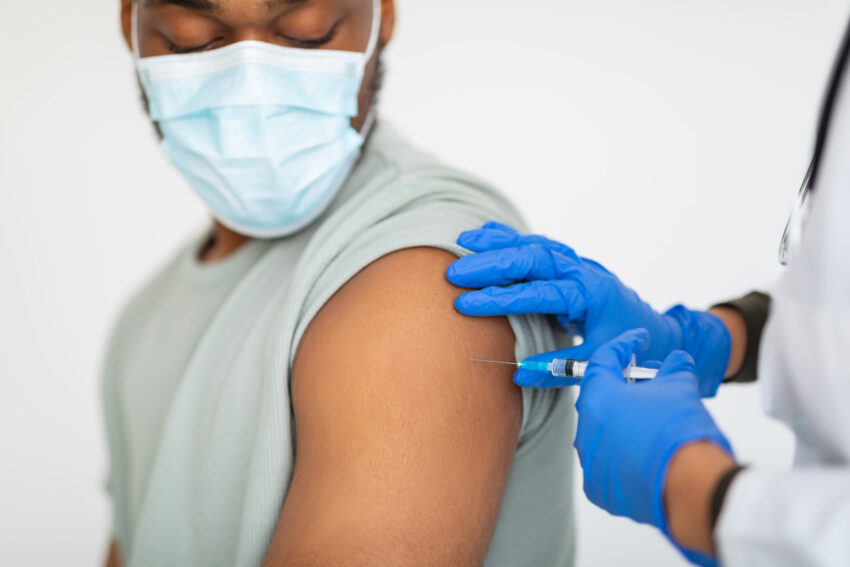
The vaccine is currently in the clinical trial phase, with 56 healthy, HIV-negative adults enrolled.
The first doses were administered in late January 2022, according to the press release.
The trial is being tested at several health centers across the country, including UT Health San Antonio.
“We seek healthy volunteers who are passionate about contributing to the science of developing an HIV vaccine,” said Barbara Taylor, assistant dean and associate professor of infectious diseases and a principal investigator on the study, according to UT Health News.
The different testing sites will study the efficacy of dosage and boosters.
“Of the volunteers, 48 will receive one or two doses of the mRNA vaccine, and 32 [volunteers of the 48] also will receive the booster. The remaining eight will receive just the booster,” according to ABC News.
Researchers will monitor participants in between doses and up until six months after their final dose.
The Impact of HIV/AIDS on Latinos
This is important because 1.3 million people in the U.S. are living with HIV.
Unfortunately, Latinos are a large percentage of them.
Latinos make up about 29% of new HIV diagnoses, despite being 18.5% of the population, according to the CDC.

Most HIV cases in Latinos are among gay and bisexual men, according to ViiV Healthcare, which published a study called Here as I Am: A Listening Initiative with Latinx Gay and Bisexual Men Affected by HIV.
There are several reasons why this disparity exists, according to Dr. Philip Ponce, medical director at Kind Clinic San Antonio.
“I think there’s a lot of cultural factors that play in. There’s still this culture of machismo, and then there are some communities that are still quite religious. Acknowledging your LGBT identity and coming to terms with it is a little bit difficult, because you have these cultural factors working against you,” Dr. Ponce said.
Lack of healthcare resources is also an issue.
“In a lot of communities, especially along the border, there’s one doctor or one clinic. And so you may not feel very comfortable, due to concern for stigma and issues around privacy, going to that clinic or going to that doctor and saying, ‘Hey, I’m gay, I need STI testing, and I want to do PrEP,’” Dr. Ponce said.
The Here as I Am report also had several key insights on how gay and bisexual Latino men are affected by HIV/AIDS:
- Family and community are central to men’s lives and identities, shaping their health and wellness for better or worse
- Interruptions in care happen for many reasons beyond men’s control
- Anti-immigrant sentiment and anti-immigrant laws have a powerful effect on men’s health
- Men want diverse and response care that reflects their needs, identity, and language
- Resilience is activated through networks and services by and for Latino men, especially youth
“The histories of Latinx communities are colorful, multifaceted and full of life and celebration. At the same time, they are complex, intersectional and influenced by many of the challenges that too often disproportionately affect communities of color,” said Guillermo Chacón, President of the Latino Commission on AIDS, according to ViiV Healthcare.
What Can You Do?
HIV and AIDS will persistently harm the Latino community unless we take action to end the stigma.
ViiV Healthcare launched an initiative called Positive Action for Latinx Men to help support those affected by HIV. Their suggestions include the following:
- Building and elevating Latino leadership in the HIV community, locally and nationally, to strengthen unity and mobilize the community to work collectively, lessening the impact that HIV has on men’s lives;
- Responding to the unique needs, identity, and language of Latino men and working with the community to promote HIV care that is diverse and responsive;
- Strengthening supportive networks for men to share their ambitions and concerns about reaching their health and wellness goals; elevating opportunities to educate around HIV; and connecting men, families, allies and communities; and
- Working to combat anti-immigrant sentiments and laws that have a powerfully negative effect on the health of Latino men living with and affected by HIV.
We can also help the work being done to promote the HIV vaccine by encouraging people to enroll in clinical trials.
Clinical trials are an important way to for researchers to create ground-breaking treatments.
But Latinos are often underrepresented in these trials, making up less than 10% of those in federal cancer and drug studies.
We need Latino volunteers for clinical trials because it helps researchers create treatments and solutions tailored for this population.
Just ask Alma Lopez.
Breast cancer is the top cause of death for Latinas, but Alma Lopez has been a breast cancer survivor for more than 15 years.
She believes participating in a clinical trial at UT Health San Antonio helped her get better treatment and better long-term health.
“Clinical trials are great for finding new treatments that help people,” Lopez said. “And it helps the scientists. It gives opportunity to better medication for all populations.”
By The Numbers
142
Percent
Expected rise in Latino cancer cases in coming years