
Share On Social!
Latinas who live on the U.S. Southwest border have more surgical infant delivery rates than their peers in the rest of the country.
Not only do those who reside on the border experience cesarean section, or C-section, more often, but Latinas have overall higher rates than white women, according to a New Mexico State University study.
This was not the case six years ago.
Jill McDonald, who serves as the director of the Southwest Institute for Health Disparities Research in the College of Health and Social Services at NMSU, told the Santa Fe New Mexican before 2013, Latinas had lower numbers than white women.
“Now, Hispanic women are more likely to have a cesarean birth than non-Hispanic white women,” McDonald said.
Maternal Disparities
Latinas already suffer from numerous pregnancy inequalities including pre-term births, maternal obesity, poor nutrition, lack of physical activity, lack of breastfeeding, and lack of paid maternity leave.
According to McDonalds’s research, this accounts for 50% of the cause behind the growing number of C-sections. The other half was attributed to:
- For-profit hospitals
- Delivery by a physician as opposed to a midwife
- Proportions of pregnancies with breech births
- Prenatal medical risk factors
- Getting prenatal care in the first trimester
McDonald also believes that cultural factors play a role as Latinas’ proximity to Mexico, which has a higher rate of C-section deliveries than the U.S., influences their decision.
Assessing the Inequities
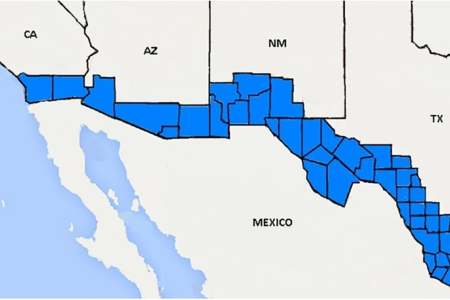
The study aimed to compare C-section delivery rates and trends on Hispanics and non-Hispanic whites in the border and non-border counties of the four states neighboring Mexico before and after 2009.
Researchers examined 187 counties in California (39.1% Latino), Arizona (31.4%), New Mexico (48.8%) and Texas (39.4%) where births occurred.
The overall C-section rate in the 23 border counties was 38.3%.
In the 164 non-border counties, the overall rate was significantly less at 30.9%. Even amongst low-risk women with no previous C-sections, 31.2% surgically delivered.
“A cesarean is good if you need it. But if it’s not necessary, both mother and baby would be better without it,” said McDonald.
“Women giving birth in high-rate counties are probably facing higher risks. And, those women will face those risks again in subsequent cesarean deliveries. After you have one, almost all women will only have cesarean deliveries for subsequent pregnancies.”
Eliminating Disparities
Reducing C-section rates is a challenge.
Several states have tested lowering reimbursements to hospitals and providers for surgical deliveries, which are more expensive than vaginal births; getting a second opinion before a C-section is a requirement in others.
“It’s not going to be one easy solution. We’re going to need a multifaceted strategy that works for women, hospitals and state legislators,” McDonald said, adding that interventions should also address cultural factors.
McDonald and her fellow researchers suggest that:
- Bilingual education in prenatal care that lays out the risk and benefits of C-sections
- Public reporting of hospital C-section rates in both English and Spanish
- Measures to remove barriers to the management of labor and delivery by doulas or certified nurse midwives.
Explore More:
AccessBy The Numbers
25.1
percent
of Latinos remain without health insurance coverage



