Share On Social!
Two reservoirs where germs can live and thrive in the human body are your blood and gastrointestinal (GI) system.
When germs spread from these reservoirs in or outside your body, it can cause harm and make you or others sick.
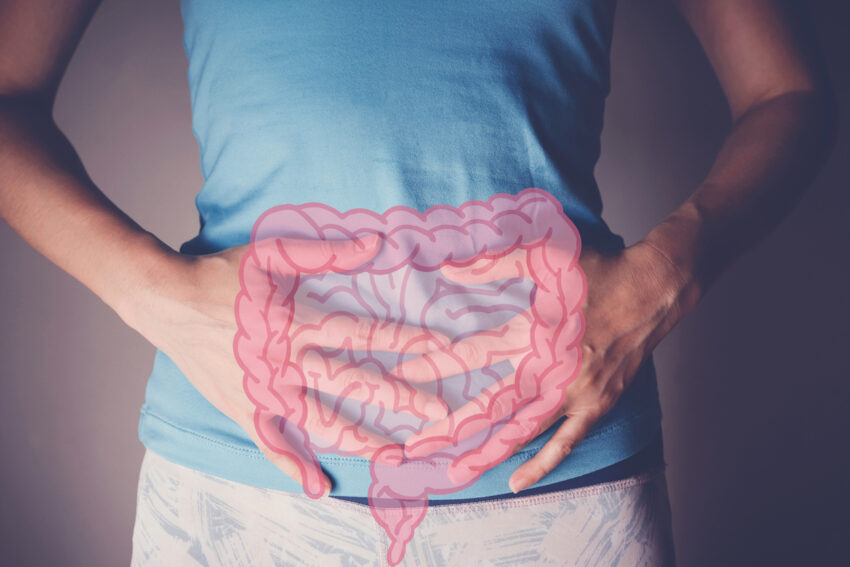
What is the Gastrointestinal System?
The gastrointestinal system or “the gut” usually refers to the lower intestine, rectum, and anus. It is part of the digestive system.
The upper GI tract, which includes the mouth, esophagus, and stomach, is also part of the digestive system. It has different types of bacteria and fungi that we usually think about separately from the gut.
The intestines are filled with bacteria and some yeasts that are an important part of a healthy immune system.
Most gut bacteria don’t cause problems in healthy people, but some germs can, such as Escherichia coli (E. coli), Klebsiella, and Proteus.
When Germs Spread from the GI System
Because germs live in the intestines, they’re in our feces, or our “stool.”
Germs in our stool travel easily from the gut to other places. It’s common to find germs from our stool in places outside of the gut, especially the skin around the groin, the hands, and the environment – like surfaces in bathrooms.
Because everyone goes to the bathroom, the germs in stool can spread onto our hands and skin when we wipe or change a diaper.
If we don’t properly wash our hands, the germs can spread to other body reservoirs, the environment, and other people, potentially making them sick.
These germs can also spread in ways we may not think about, like flushing toilets.
Germs Can Spread from Your Blood
Unlike other parts of the body, blood is not supposed to have germs at all.
However, some viruses are “bloodborne” and can get into your blood. When this happens, the virus can cause an infection and spread to other people.
Some examples of bloodborne viruses are HIV, Hepatitis B, and Hepatitis C.
The most common way that bloodborne viruses spread in healthcare is when an infected person’s blood is on a sharp item that causes a break in someone else’s skin, such as a needlestick. When this happens, the infected blood can enter the body, causing a new infection.
Additionally, if a needle or syringe is reused on more than one patient, or a vial of medication gets contaminated with blood, germs in one person’s blood could spread to another.
Skin that is cut or damaged in other ways, like from eczema, is also vulnerable to bloodborne viruses.
What Can You Do to Promote Infection Control in Your Healthcare Setting?
It is important to protect yourself, patients, and colleagues from germs that can spread from the GI system and blood.
Remember to properly clean your hands and wear appropriate PPE, such as gloves.
Access more information about infection prevention and control in healthcare by visiting resources from CDC Project Firstline.
Project Firstline creates resources, including videos and shareable images, web buttons, posters, and print materials. They also have facilitator toolkits to help workers lead trainings even if they are not an infection control expert.
Salud America! at UT Health San Antonio is working with the National Hispanic Medical Association to bring Project Firstline infection control educational content to healthcare workers, so they are equipped with the knowledge they need to protect themselves, their facilities, and their patients (Latinos and all communities) from infectious disease threats in healthcare settings.
You can read these articles:
- What is Project Firstline?
- What’s a Virus?
- How Do Viruses Make Us Sick?
- What is Ventilation and Why Does It Matter?
- What’s a Respiratory Droplet and Why Does It Matter?
- Why Do Cleaning and Disinfection Matter in Healthcare?
- We Need to Talk about Hand Hygiene Again
- What is the Goal of Infection Prevention and Control in Healthcare Settings?
- N95 Respirators: Everything You Need to Know
- How Do I Safely Use a Multi-Dose Vaccine Vial?
- Why are Gowns, Gloves, and Eye Protection Recommended for COVID-19?
“Healthcare teams in hospitals, nursing homes, and other care settings are the front lines against the spread of infection,” said Dr. Amelie G. Ramirez, director of Salud America! at UT Health San Antonio. “CDC’s Project Firstline is bolstering those efforts by developing evidence-based tools that can be delivered in a variety of ways to make infection control learning convenient and accessible for busy healthcare staff.”
Learn More about Project Firstline!
Explore More:
Infection ControlBy The Numbers
142
Percent
Expected rise in Latino cancer cases in coming years




[…] The pandemic is another chapter in the bitter story of American racism and inequality. Black and Latinx people are being infected and are dying at much higher rates than white Americans. Many people of […]
[…] coronavirus has killed over 61,000 Latinos in America according to the CDC, accounting for over 18.2% of the total COVID deaths in the […]
[…] Whereas Hispanics make up 11% of D.C.’s inhabitants, they signify 19% of the COVID cases, and 14% of the deaths. Equally, 46% of D.C.’s residents are Black, they usually make up an alarming 75% […]
[…] and historical mistreatment. According to the U.S. Centers for Disease Control and Prevention, Latino and Black American communities are three times more likely to become infected with […]
[…] Covid pandemic has hit the Latino community particularly hard, and data from the nonprofit health equity advocacy group Salud America! shows Latinos lead in the 0-24 age […]
[…] the pandemic, Latinos took major blows, both in terms of COVID-19 cases and also from the economic recession under former President Donald Trump. Nearly half (49%) of […]
[…] the positive trend, the harm may have already been done. The pandemic has disproportionately impacted Latino communities. Reuters reported that election-related or political disinformation that […]
[…] pesar de la tendencia positiva, es posible que el daño ya esté hecho. La pandemia ha impactado desproporcionadamente Comunidades latinas. Reuters informó que la desinformación política o relacionada con las […]
[…] residentes blancos muestran una tasa mucho más baja con 10 muertes por cada 100,000 habitantes(8 9) . Los afroestadounidenses por su parte, denuncian subsistemas de salud que les segregan […]
[…] https://salud-america.org/coronavirus-case-rates-and-death-rates-for-latinos-in-the-united-states/ […]
[…] https://salud-america.org/coronavirus-case-rates-and-death-rates-for-latinos-in-the-united-states/ […]
[…] communities have the second-highest number of COVID-19 cases in the U.S. They’re also more likely to become hospitalized and die from the disease than other […]
[…] total, around 160,000 Latinos were killed by COVID-19. This accounts for 16% of the 1 million deaths in the country. The […]