
Share On Social!
Latinos are more likely than their peers to have mental health issues, which usually go unaddressed and untreated, according to a Salud America! research review.
And with today’s anti-immigrant climate, the mental health of Latinos continues to suffer. Fear of deportation, mainly those in immigrant communities, is one of the main reasons mental health goes untreated.
But there’s good news!
Researchers at Massachusetts General Hospital’s Disparities Research Unit have tested a novel preventive intervention designed to provide tailored treatment for Latino immigrants with both mental health and substance misuse symptoms, according to a press release. This research is a collaboration between teams in Spain, U.S. and Puerto Rico.
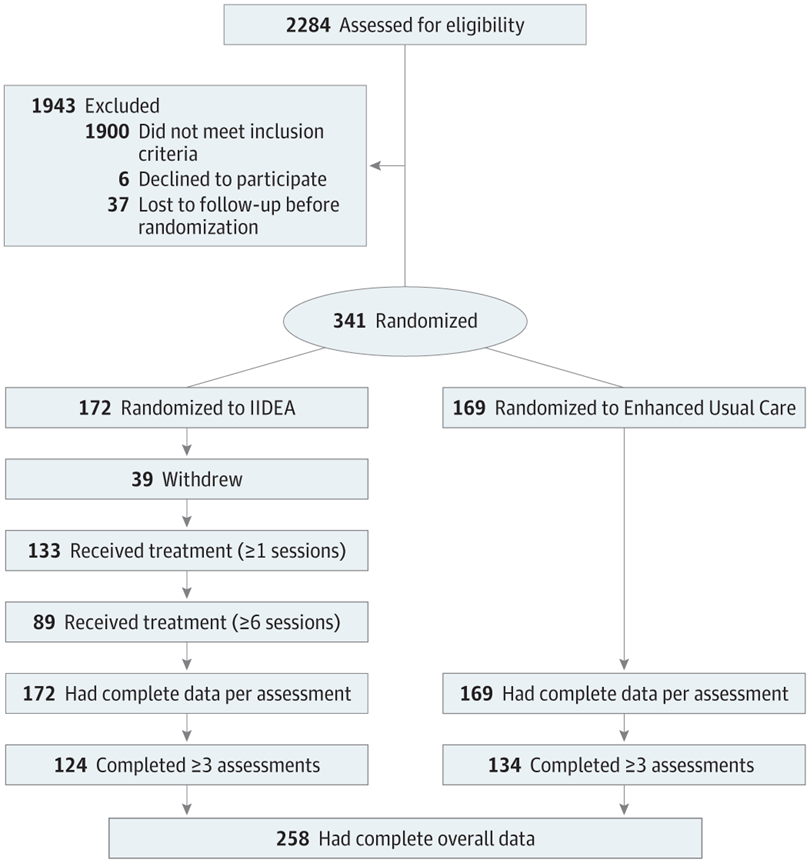
IIDEA indicates Integrated Intervention for Dual Problems and Early Action. Source: JAMA Open Network
“We know that Latino patients benefit when treatments are culturally tailored, evidence based and accessible,” Margarita Alegria, PhD, chief of the Disparities Research Unit and a professor in the Departments of Medicine and Psychiatry at Harvard Medical School, told News Medical. “We sought to provide a customized treatment to Latino immigrants in different contexts—in the U.S. and Spain—to see how best to serve this growing and important demographic population in our communities.”
New Research & Treatment
The researchers established the Integrated Intervention for Dual Problems and Early Action (IIDEA) program to provide culturally tailored care that incorporates evidence-based practices. This consists of cognitive restructuring and mindfulness, as well as with substance-craving reduction and coping strategies.
As stated in the news release, IIDEA is an integrated therapy that involves 10-12 weekly sessions that include motivational interviewing, cultural formulation, assessment of barriers to care, psychoeducation, cognitive behavioral therapy, mindfulness exercises, communication skills and reduction of risk behaviors.
This program was offered to Latino adults ages 18-70 in the Greater Bostons area, as well as Madrid and Barcelona, Spain. This cohort was screened positive for co-occurring symptoms.
The cohort was individually identified by a bilingual/bicultural staff across primary care and emergency department sites, along with non-clinical settings like Latino-serving community-based organizations. 341 participants were randomized to receive either the IIDEA intervention or take part in an enhanced usual care group with regular telephone check-ins to assure safety. Participants were assessed on enrollment and 2, 4, 6, and 12 months after enrollment.
The results indicated that the intervention reduced mental health symptoms.
Secondary analyses showed that participants who initially screened with moderate to severe symptoms, IIDEA was effective in reducing both substance use and mental health symptoms.
Additionally, participants who partook in four or more sessions saw decreasing drug use and mental health symptoms.
“These results point to the potential for an adequate dose of tailored therapy, even as few as four sessions, to improve outcomes for those with moderate to severe symptoms,” Alegria said.
By The Numbers
44
million
immigrants live in the United States



