
Share On Social!
Minorities who visit an emergency room in the U.S. are less likely to receive prescriptions for certain medications than Whites, according to a new study.
Researchers found that Latinos and Blacks specifically face disparities in obtaining analgesics, which include a wide range of pain killers. The study also noted that other minority communities might undergo similar experiences, but further research is needed in the topic.
“The reasons for these disparities are likely complex and multifold and may include factors such as implicit bias, language barriers, and cultural differences in the perception and expression of pain and institutional differences in ERs that serve mostly Black and Hispanic patients,” Dr. Andrew Meltzer, senior author of the study and a researcher at George Washington University School of Medicine & Health Sciences, told Reuters.
Inequity in Perscriptions
Scientists conducted a systematic review and analyzed data from 14 previously published studies of pain management in American emergency rooms (ERs) that, in total, included 7,070 white, 1,538 Latino, and 3,125 black patients.
Their analysis found that when compared to Whites:
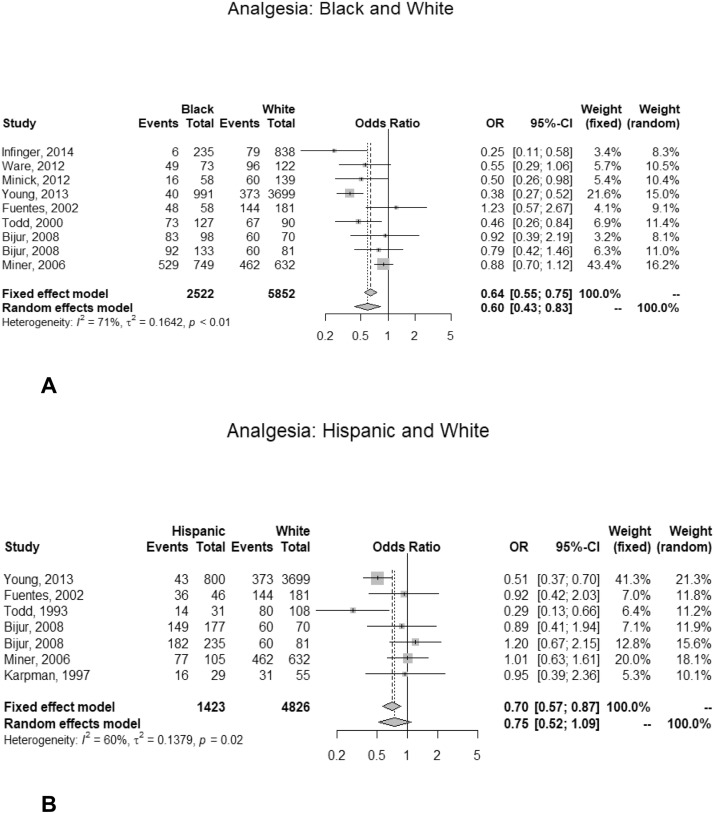 Black patients were 40% less likely to receive medication to alleviate acute pain
Black patients were 40% less likely to receive medication to alleviate acute pain- Latino patients were 25% less likely to receive medication to alleviate acute pain
- Black patients were 34% less likely to receive opioids for acute pain
- Latino patients were 13% less likely to get opioids for acute pain
Worse, those numbers have a variety of adverse impacts on these communities.
“Unrelieved pain can lead to a wide range of consequences such as growing distrust towards physicians and the medical community, economic burden from its debilitative effects, and physical and emotional repercussions,” Meltzer said.
“Given the current opioid epidemic, however, it remains unclear if more pain medicine should be a marker of higher quality care.”
However, the study does come with some limitations, including:
- That the study was not controlled
- A Lack of data on the number of pain patients experienced
- Differences on how much pain was reported
- Lack of data on health outcomes
“Delayed pain relief may lead to poor healing or prolong the healing,” Dr. Carmen Green, a professor of anesthesiology at the University of Michigan schools of medicine and public health in Ann Arbor, told Reuters.
“In addition, there are psychological, implications ranging from suffering to fear all the way to PTSD,” said Green, who wasn’t involved in the study but does research in this issue. “Let us not forget pain has been used to torture.”
Racism in Healthcare
Implicit bias in healthcare settings is nothing new.
Research shows that physicians and other healthcare professionals are frequently susceptible to their unconscious bias, or otherwise known as implicit bias — automatic processing that is influenced by stereotypes, which then impact actions and judgments.
Data also shows that White male physicians are less likely to prescribe pain medications to black patients than white patients.
Moreover, Latino men are much less likely to receive optimal treatment for high-risk prostate cancer than White men due to this kind of systematic racism.
Yet, research also shows that Latinos and other minority patients have positive health outcomes with doctors who look like them. Unfortunately, Latinos and other minorities are incredibly underrepresented in the medical field.
Reducing Prejudice in Medicine
Implicit bias has severe consequences for Latinos and other peoples of color.
Still, there are many ways to overcome this issue, including teaching cultural competencies that can improve healthcare outcomes, reducing the cost of care, and producing more Latino and black doctors.
“We tend to be more sympathetic to those who look like us,” Green said.
“Overall, racial and ethnic minorities tend to receive lesser quality of care, have lesser quality health insurance, have decreased access to care, and experience diminished outcomes that lead to disparities.”
How Can You Tackle Implicit Bias?
Seek training or help put an end to microaggressions.
You can also “rewire” implicit bias toward more compassion for others.
Download the free Salud America! “Find Out If You Have Implicit Bias and What to Do Next” Action Pack. This will guide you to see if you have implicit bias, reflect and learn from others who have overcome their own implicit bias, and encourage others to learn about implicit bias, too.
The Action Pack was created by Dr. Amelie G. Ramirez, director of Salud America! at UT Health San Antonio.
Explore More:
Increasing RecognitionBy The Numbers
3
Big Excuses
people use to justify discriminatory behavior



