Share On Social!
Children don’t magically “get over” trauma when they turn 18.
Trauma, toxic stress, and adverse childhood experiences permanently change a child’s body and brain, which can have serious, lifelong consequences, according to a recent report from the Center on the Developing Child at Harvard University.
Here are four ways trauma can overload a child’s developing system:
1. Hormone level changes: Cortisol and adrenaline are the “stress hormones” that help you react to a perceived threat or danger by directing blood flow to major muscle groups and bypassing the thinking part of the brain to activate the survival part.
- High levels of these hormones keep your blood pressure elevated, which weakens the heart and circulatory system; keep your glucose levels elevated, which can lead to type 2 diabetes; and disrupt your immune system and inflammatory response system, which can lead to lupus, multiple sclerosis, osteoporosis, abdominal obesity, and depression, and reduce your ability to fight infection.
- Hormone level changes early in life when brain development is most rapid can have a drastic impact on brain architecture and function, as well as other organs, thus lifelong physical and mental health problems.
2. Immune system changes: Through multiple organs, tissues, and cells, the immune system defends against infections, allergies, and inflammatory reactions.
- Trauma is linked to thymus involution, atrophy of the spleen and lymph nodes, telomere shortening, and increased stress hormones, which impairs immunity and increases inflammation.
- Impaired immunity and inflammation increase risk for cancer, cardiovascular disease, diabetes, anxiety, depression, viral infections, autoimmune diseases, allergies, and asthma.
3. 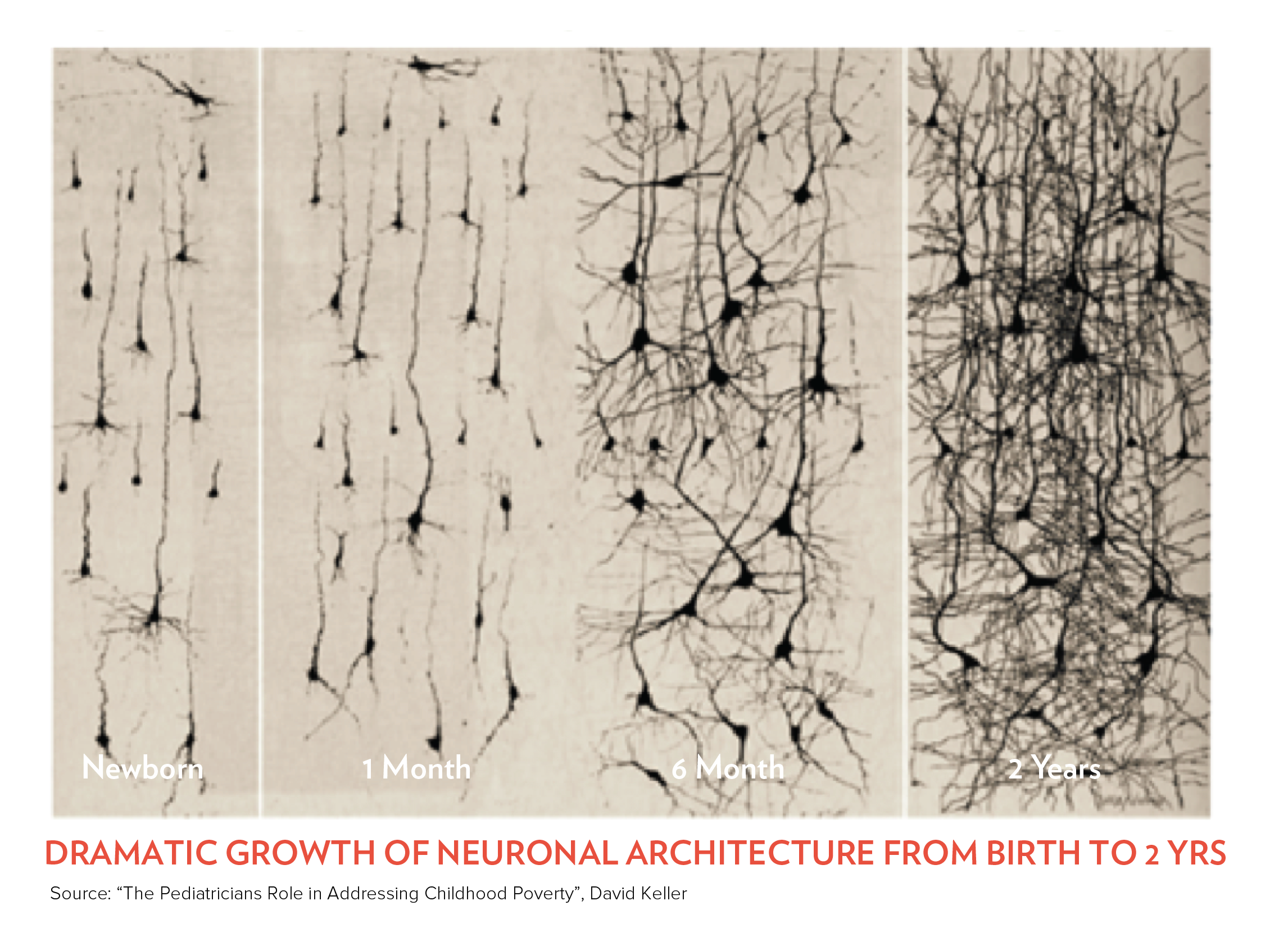 Neurological changes: We are born with 100 billion neurons—brain nerve cells—which are almost all of the neurons we will ever have. The connections between neurons develop vision, hearing, language, and higher cognitive functioning.
Neurological changes: We are born with 100 billion neurons—brain nerve cells—which are almost all of the neurons we will ever have. The connections between neurons develop vision, hearing, language, and higher cognitive functioning.
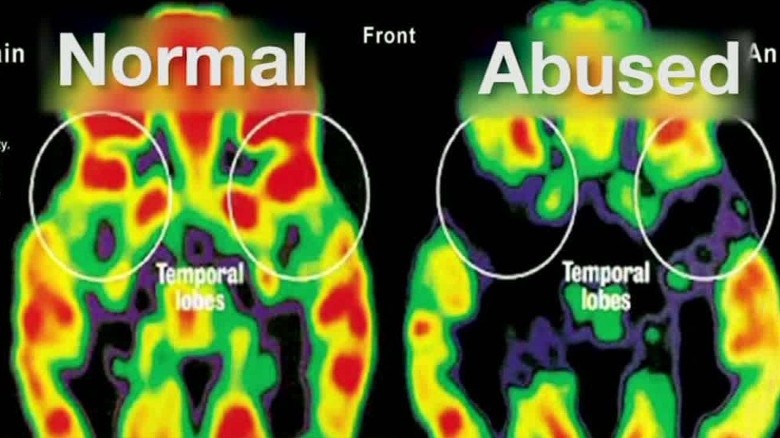
- The prolonged activation of stress hormones in early childhood can reduce neural connections in the thinking area of the brain dedicated to learning and reasoning, thus limiting cognitive ability.
- Continuous trauma can weaken remaining neural pathways to the thinking part of your brain and strengthen neural pathways to the survival part, thus bypassing the thinking part, which makes some children less capable of coping with adversity as they grow up.
4. Epigenetic changes: Epigenetics is the study of how your environment and experiences can alter which genes turn on and off, known as gene modification. For example, “you may be born with a capacity to be tall and confident, but if you are undernourished and abused as a child, you are likely to turn into a stunted and fearful adult instead,” according to Dr. John Launer.
- Trauma can induce epigenetic changes for genes related to mental health, obesity, drug addiction, immune function, metabolic disease, and heart disease.
Sadly, policies that affect young children generally do not address the severity to which early exposure to trauma and stress can affect a child’s body and brain.
So what can we do?
The presence of a stable caregiver can regulate these changes in the early years and help children better cope with adversity when they grow up.
Public policy and private sector actions can prevent childhood trauma, reduce potential damage, promote greater resiliency, and improve physical and mental health. Consider these six implications for policy and practice from the experts at the Center on the Developing Child at Harvard University.
One recommendation—which is supported by the findings of a Salud America! research review on Latino childhood development—suggests “high-quality early care and education programs that provide stable, supportive relationships with caring adults should be more available to young children who are at risk of experiencing tolerable or toxic stress.”
“Assuring that a young child has reliable, safe, and engaging relationships both at home and in out-of-home care can buffer the effects of multiple stressors that may exist in his or her life,” according to the Harvard report.
Sign up for the Salud America! “Trauma Sensitive School Action Pack.” It is a free guide with coaching to help school personnel talk to decision-makers, build a support team, craft a system to identify and support traumatized students, and more!
Or sign up for the free Salud America! “Handle With Care Action Pack” to start a Handle With Care program, in which police notify schools when they encounter children at a traumatic scene, so schools can provide support right away.
By The Numbers
28
percent
of Latino kids suffer four or more adverse childhood experiences (ACES).



