
Share On Social!
Cancer, mortality rates continue to decline for men, women, and children, according to an annual report released by the National Institutes of Health.
Great news, right? Not so fast.
In a special section of the report, researchers found that cancer development and mortality rates increased between 2011 and 2015 for women ages 20 to 49 — whereas men, who historically have higher rates than women, did not experience such gains.
The data also shows continuing disparities among Latinos and other racial/ethnic populations.
“We are encouraged by the fact that this year’s report continues to show declining cancer mortality for men, women, and children, as well as other indicators of progress,” said Betsy A. Kohler, executive director of North American Association of Central Cancer Registries (NAACCR), in a press release.
“There are also several findings that highlight the importance of continued research and cancer prevention efforts.”
Cancer & Mortality Rates
Overall, the report—a collaborative effort of the National Cancer Institute, the National Institutes of Health, the Centers for Disease Control and Prevention (CDC), the American Cancer Society, and NAACCR— shows that all combined cancer sites and deaths continued to decline from 1999 to 2016.
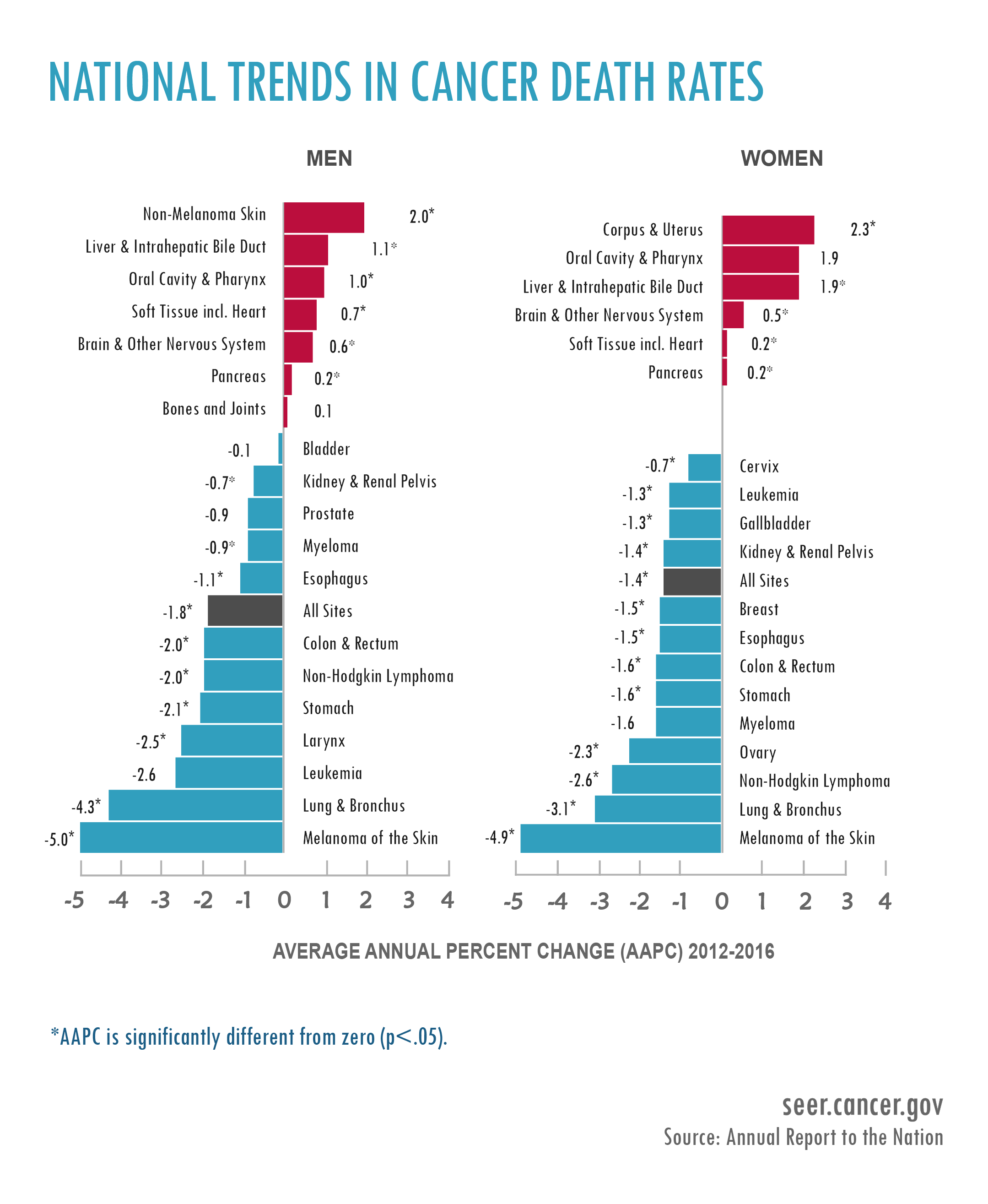 From 2012 to 2016, rates decreased about an average of 1.8% per year in men and 1.4% per year in women.
From 2012 to 2016, rates decreased about an average of 1.8% per year in men and 1.4% per year in women.
The most common cancers for men were:
- Colon
- Testicular
- Melanoma
The most common cancers for women were:
- Breast (far exceeding any of the other cancers)
- Thyroid
- Melanoma
New cases of, deaths from lung, bladder, and larynx cancers continue to decrease due to various factors, such as a long-term decline in smoking, according to the research.
However, rates of cancers associated with obesity and physical inactivity are on the rise.
This is especially true if you are between the ages of 25-49, as your risk of getting obesity-related cancer has increased. Rates of uterine, post-menopausal breast, and colorectal cancers also showed increases among that demographic.
Unexpected Discoveries
The special section of the reports shows that rates for cancer development and deaths were more prevalent among women rather than men, who historically have higher rates in most cases.
The average annual incidence rate for all combined cancer sites was about 1.2 times higher among men than among women from 2011 to 2015. Moreover, the average yearly death rate from 2012 to 2016 among men (all ages) was 1.4 times the rate among women.
Yet, researchers found that both incidence and death rates were higher among women between ages 20 to 49.
“The greater cancer burden among women than men ages 20 to 49 was a striking finding of this study,” said Dr. Elizabeth Ward, lead author of the study and a consultant at NAACCR.
“The high burden of breast cancer relative to other cancers in this age group reinforces the importance of research on prevention, early detection, and treatment of breast cancer in younger women.”
Racial and Ethnic Disparities
Latinos and other minorities have always disproportionally faced a plethora of disparities in incidence and mortality rates of certain cancers such as liver, cervical, and rare cancers, compared to their white counterparts.
The study illustrates further disparities. Latinas, along with black women, had the highest mortality rate for leukemia. Furthermore, Latino men had the highest mortality rate for leukemia and stomach cancer.
Moreover, men’s death rates decreased in 10 of the most 19 cancers. Six cancer did see an increase, including liver, oral cavity, pharynx cancer, and melanoma.
For women, death rates for 13 of the 20 most common cancers also decreased but increased for five. The highest increase was also liver cancer, and uterine was a significant form as well.
Liver cancer disproportionally affects Latinos, especially those in South Texas. Risk factors may include:
- diabetes and obesity
- hepatitis
- genetic predisposition
- environmental contamination and hazards along the Texas-Mexico border, such as aflatoxin exposure.
Additionally, melanoma is continuously rising in the Latino population. In the past 20 years, the rate melanoma – the most dangerous form of skin cancer – has increased by 20%.
“Major declines overall in cancer mortality point in the right direction, yet significant differences remain in cancer cases and deaths based on gender, ethnicity, and race,” said CDC Director Dr. Robert R. Redfield. “A better understanding of these discrepancies improves cancer diagnosis and recovery for all patients and is vital to our public health mission.”
Explore More:
AccessBy The Numbers
142
Percent
Expected rise in Latino cancer cases in coming years



