
Share On Social!
The way you eat can have a significant impact on your overall health.
Food choices can even be the cause of developing invasive cancers, according to a new study published in the Journal of the National Cancer Institute Cancer Spectrum. Researchers found that individual diets could play a factor in 80,110 of the newly reported invasive cancer cases in 2015.
That’s 5.2% of the total number of cases among U.S. adults from that year.
“Our findings underscore the opportunity to reduce the cancer burden and disparities in the United States by improving food intake,” said Dr. Fang Fang Zhang, one of the study’s authors and a cancer, nutrition researcher at Tufts University.
About the Study
Researchers analyzed nationally-representative information to identify trends between cancer development and diet. Specifically, their data stems from risk estimates of diet and cancer relations from the World Cancer Research Fund International (WCRF) and the American Institute for Cancer Research (AICR). 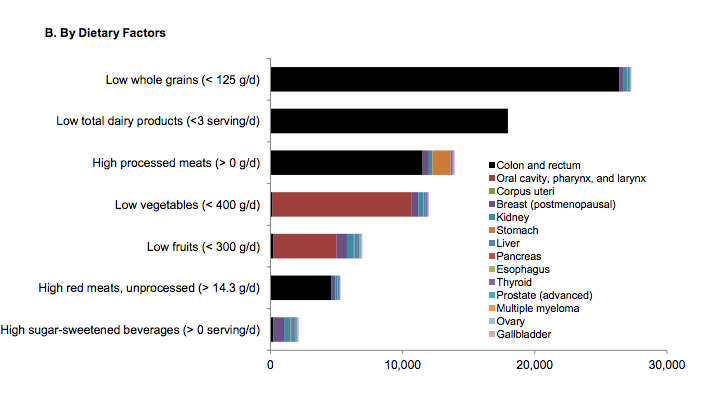
They estimated the annual number and proportion of new cancer cases attributed to suboptimal intakes of 7 dietary factors among US adults ages 20 years and older as well as population subgroups.
Based on that data, they estimated the number of new cancer cases they could attribute to inadequate intake of seven different dietary factors, including meats, vegetables, dairy, and grains.
The results showed that over 80,000 new cancer cases are likely linked to poor nutrition.
Researchers attributed more than 67,000 of these cases to direct diet associations and over 12,000 to obesity-mediated links.
Colon cancer had the most significant link to diet-associated cancer cases (38.3%).
This issue should be concerning to Latinos and other minority groups.
Latinos, Blacks, and middle-aged men (45-64 years) had the highest proportion of diet-related cancer burdens than any other demographic group.
These overall rates are comparable to the cancer burden associated with alcohol, which is 4% to 6%. However, excessive body weight is associated with 7% to 8% of the cancer burden, and physical inactivity is associated with 2% to 3%.
Overall, a diet with low consumption of whole grains and dairy products and high consumption of processed meats contributed to the highest cancer burden.
Latinos, Diet, & Cancer
The study found that Latinos and Blacks had a greater diet-related cancer burden when compared to their white counterparts.
Diet
An unhealthy diet is already a leading factor in causes of death, with more than 500,000 fatalities attributed to poor nutrition.
Sadly, fast food and corner stores outnumber supermarkets and farmers’ markets in many Latino neighborhoods, according to a Salud America! Research Review.
Latinos also tend to be a younger population with higher rates of obesity. Not only do they struggle with local access to healthy food, but also safe places to play.
Obesity & Cancer
Unfortunately, Latinos and other minorities have always disproportionally faced countless cancer disparities. They experience higher rates of incidence and mortality in cancers such as liver, cervical, and rare cancers, compared to their white counterparts.
A recent study showed that Latinas, along with black women, had the highest mortality rate for leukemia. Additionally, Latino men had the highest mortality rate for leukemia and stomach cancer.
Furthermore, Latino and black children are more likely to die of childhood cancers more often than their white counterparts, including preventable and treatable forms.
“Our results call for nutrition policies to address the U.S. cancer burden,” said the study authors, who proposed putting government-sponsored warning labels on red meats and other cancer-linked foods.
Explore More:
Healthy Neighborhoods & CommunitiesBy The Numbers
1
Supermarket
for every Latino neighborhood, compared to 3 for every non-Latino neighborhood



