
Share On Social!
While the elderly are highly susceptible to the coronavirus COVID-19, young adults aren’t off the hook, either.
Almost 40% of U.S. coronavirus patients who were sick enough to need hospitalization were between the ages of 20 to 54, according to recent CDC data.
“There seems to be this ethos that the virus is no big deal for young people,” said Dr. Mark Pasternack, chief of the pediatric infectious disease unit at Massachusetts General Hospital, told the Newbury Press. “But it is a big deal because some young people are getting very sick and because they are also very serious vectors of disease spread.”
Why Obesity and Coronavirus Outbreak is a Concern for Young People in the U.S.?
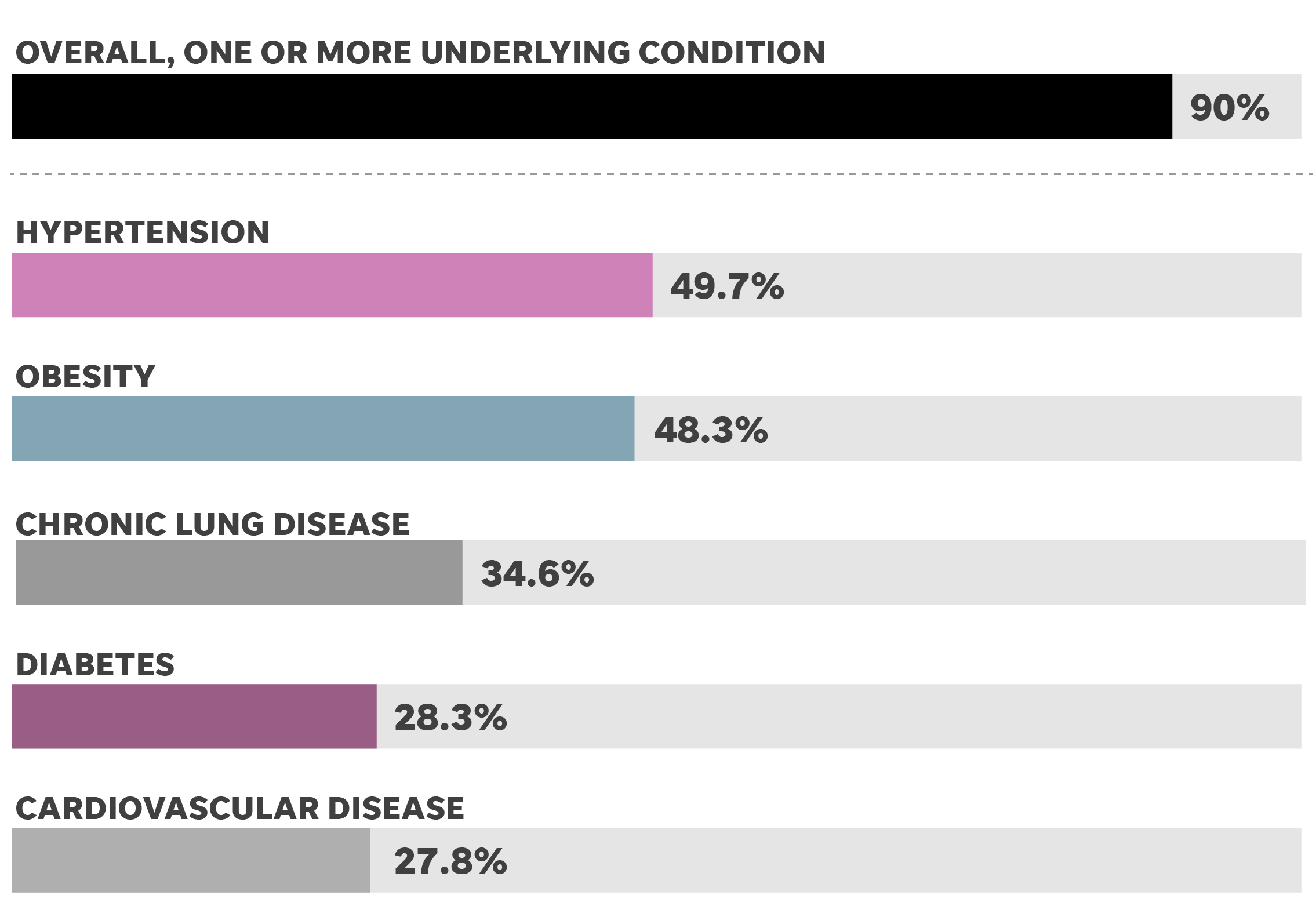
Obesity may be one of the most important predictors of severe coronavirus illness among young patients, new data from the NYU School of Medicine suggests.
The study showed that people with a BMI above 40 were six times more likely to require hospitalization. Worse, many younger patients experiencing severe COVID-19 symptoms were healthy but were suffering from obesity.
Chronic inflammation is usually present in people with obesity. It can weaken the immune system. It also can impair the healing process and prolong recovery.
Mainly, the coronavirus outbreak is more severe in adults, especially those with weak immune systems, according to a recent World Health Organization (WHO) report.
In the U.K., of the first 2204 patients admitted to 286 NHS ICU’s with COVID- 19, 72.7% of them had overweight or obese, according to a recent study analyzing the hospital’s data.
Obesity is often linked to other health issues, such as hypertension, diabetes, and heart disease — which could also be risk factors for COVID-19 — this new research points to the condition itself as the issue.
Many others suggest that obesity, type 2 diabetes, and a cluster of risk factors all linked to poor diet is the root cause behind increased mortality from COVID -19.
Unfortunately, obesity in people under 60 years is a newly identified epidemiologic risk factor, according to the NYU study. This may contribute to increased COVID-19 morbidity rates experienced in the U.S.
Obesity and Health Equity
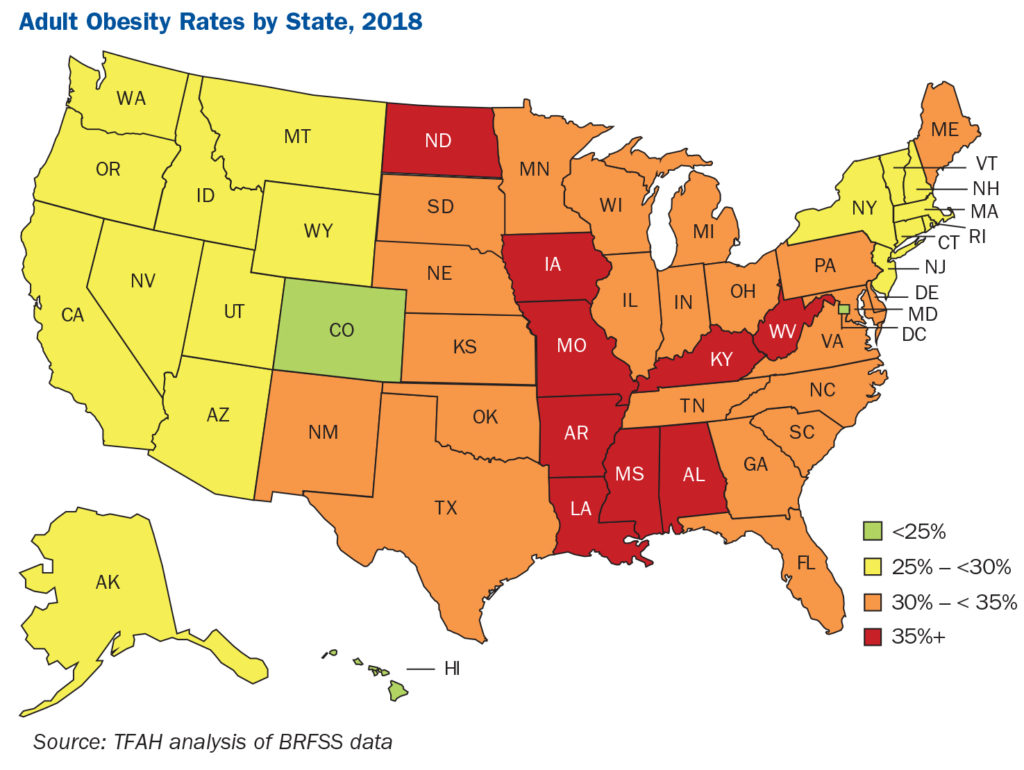
The United States has one of the highest obesity rates in the world.
Adult obesity rates went above 35% in 2018—a historic level of obesity in the U.S.—according to the new State of Obesity report by Trust for America’s Health. Worse, there was an increase in seven states from 2017.
As of 2015-2016, nearly half of Latino (47%) and Black adults (46.8%) had obesity while adult obesity rates among White and Asian adults were 37.9 percent and 12.7 percent, respectively.
“[Young people] are not immune to risk just because they are young,” Dr. Clyde Yancy, a professor and chief of cardiology at Northwestern University’s Feinberg School of Medicine, told the Herald-Mail. “Once hypertension is present, once obesity is present, and especially this preexisting cardiovascular disease, irrespective of age, there’s a higher risk, and the California Department of Health data seemingly are bearing that out.”
Obesity levels are closely tied to social and economic conditions and that individuals with lower incomes are more at risk.
More than one-third of U.S. high-school students had overweight or obesity, including a higher rate among Latinos (37.7%) than their black (36%) and white (26.5%) peers, according to CDC data.
Salud America! research shows that U.S. Latinos face inequities in many areas from poverty and social support.
The COVID-19 outbreak adds to the problem and contributes to disparities in health and wealth, mainly among Latinos.
Hence, beyond developing equitable practices in testing, tracking, and treating COVID-19, local and state leaders must develop programs to fix the long-term social, economic, and health inequities.
Learn more about the coronavirus outbreak and its implications concerning health.
By The Numbers
25
years
of life expectancy between some U.S. cities.



