Share On Social!
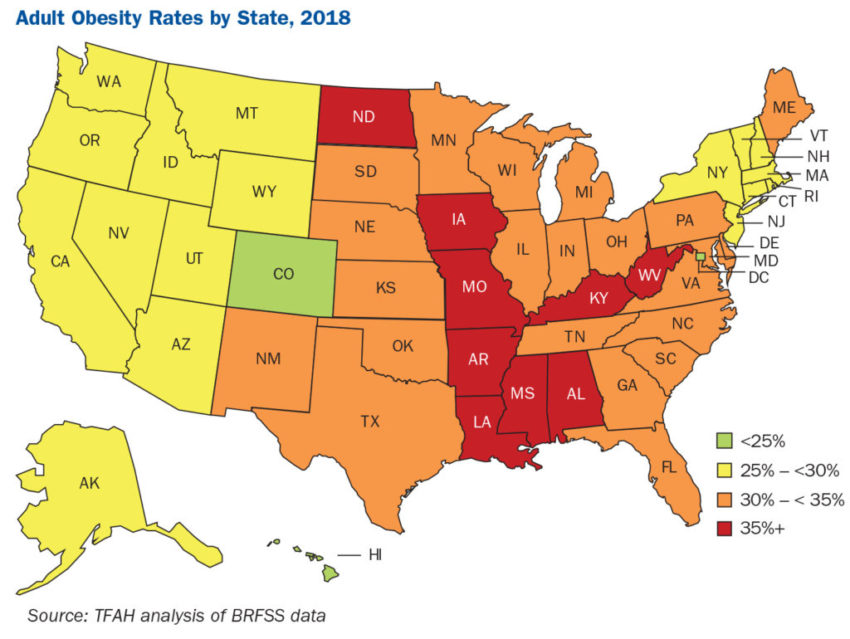
Nine U.S. states had adult obesity rates above 35% in 2018, up from seven states at that level in 2017, an historic level of obesity in the U.S., according to the new State of Obesity report by Trust for America’s Health.
In 2012, no state had obesity rates over 35%.
This alarming rise is even worse among Latinos.
Data indicate that 47% of Latino adults and 25.8% of Latino children had obesity—the highest combined obesity rate among all racial/ethnic groups.
“These latest data shout that our national obesity crisis is getting worse,” said John Auerbach of Trust for America’s Health. “They tell us that almost 50 years into the upward curve of obesity rates we haven’t yet found the right mix of programs to stop the epidemic.”
Alarming Rise in Obesity Rates
The State of Obesity report, supported by the Robert Wood Johnson Foundation, examines CDC data to provide an annual snapshot of obesity rates nationwide.
Last year, seven states had adult obesity rates higher than 35%.
This year, that number rose to nine—Alabama, Arkansas, Iowa, Kentucky, Louisiana, Mississippi, Missouri, North Dakota and West Virginia.
 Here are the states with the highest rates:
Here are the states with the highest rates:
- 39.5%, Mississippi (3.4% Latino population)
- 39.5%, West Virginia (1.7% Latino population)
- 37.1% Arkansas (7.7% Latino population)
- 36.8% Louisiana (5.2% Latino population)
- 36.6%, Kentucky (3.8% Latino population)
Here are the states with the lowest rates:
- 23%, Colorado (21.7% Latino population)
- 24.7%, Washington, D.C. (11.3% Latino population)
- 24.9%, Hawaii (10.7% Latino population)
- 25.7%, New Jersey (20.6% Latino population)
- 25.7%, Massachusetts (12.3% Latino population)
In all, 33 states had statistically significant increases in their rates of adult obesity between 2013 and 2018.
Big Obesity Rates among Latinos
The report highlights that people with lower incomes and social and economic barriers are at higher risk for obesity.
 Latinos also had higher risk for obesity:
Latinos also had higher risk for obesity:
- Nearly half of Latino (47%) and Black adults (46.8%) had obesity. Only 37.9% of White adults did.
- Obesity rates also were higher among Latino (25.8%) and Black children (22%). Only 14% of White children did.
- Latino youth especially struggle with obesity.
- Obesity variation exists between Latina men and women (more among women).
- Variation also exists among Latino ethnicity (more among Puerto Ricans and Mexicans).
Why the higher risk?
Poverty and food swamps are prolific in Latino neighborhoods. Fast food outnumbers supermarkets and farmers’ markets, according to a Salud America! Research Review.
Latinos also face marketing of junk food and less access to recreational spaces.
“To an increasing degree, overweight, obesity, and sugary diets are driving up health care costs and are costing Americans years of healthy life,” said Dr. Christopher Murray of University of Washington in a past study.
Why Do Obesity Rates Matter?
Obesity has serious health consequences.
These include increased risk for diabetes, high blood pressure, and many types of cancers.
Obesity also is estimated to increase national healthcare spending by $149 million annually. Being overweight or obese is the most common reason young adults are ineligible for military service.
“Our report highlights the fundamental changes that are needed in the social and economic conditions that make it challenging for people to eat healthy foods and get sufficient exercise,” Auerbach said.
What Could Work to Reduce Obesity Rates?
The good news is that obesity is declining for children enrolled in WIC (Special Supplemental Nutrition Program for Women, Infants and Children). The rate fell from 15.9% percent in 2010 to 13.9% in 2016, even though Latino children in the program still had higher rates than their Black and White peers.
 “In 2009, the USDA updated WIC food packages to more closely meet recommended national dietary guidelines including the addition of more fruits, vegetables and whole grains and reduced fat levels in milk and infant formula,” according to the report.
“In 2009, the USDA updated WIC food packages to more closely meet recommended national dietary guidelines including the addition of more fruits, vegetables and whole grains and reduced fat levels in milk and infant formula,” according to the report.
The report also makes 31 other recommendations to reduce obesity:
- Increase the price of sugary drinks, using actions like the sugary drink taxes in Berkeley, Calif., and Philadelphia.
- Expand WIC to age 6 for children and for two years postpartum for mothers. Fully fund the WIC breastfeeding Peer Counseling Program.
- Make it more difficult to market unhealthy food to children by ending federal tax loopholes and business costs deductions related to the advertising of such foods to young audiences.
- Fully fund the Student Support and Academic Enrichment program and other federal programs that support student physical education.
- Encourage safe physical activity by funding Safe Routes to Schools (SRTS), Complete Streets, Vision Zero and other pedestrian safety initiatives through federal transportation and infrastructure funding.
- Strengthen and expand school nutrition programs beyond federal standards.
- Enforce existing laws that direct most health insurers to cover obesity-related preventive services at no-cost sharing to patients.
People can also speak up against cuts in food aid programs, like SNAP.
“Policies such as these are proving effective in changing behavior,” Auerbach said. “But, no single solution – however promising – is sufficient. Obesity is a complex problem and will need multi-sector, multi-factor solutions.
By The Numbers
142
Percent
Expected rise in Latino cancer cases in coming years



