
Share On Social!
There is a shortage of mental health professionals in the United States.
 This situation is more severe for Latino and other minorities, who face barriers of language and culture that can make it hard to seek and get help, Pew Charitable Trusts reports.
This situation is more severe for Latino and other minorities, who face barriers of language and culture that can make it hard to seek and get help, Pew Charitable Trusts reports.
Take, for instance, Ana Paula Guerrero of Aurora, Ill.
Guerrero says it makes it easier and better for her therapy if she doesn’t have to translate her emotions from her native Spanish to her adopted English.
“When I am talking about certain feelings in Spanish, it’s (about) vocabulary and being able to gather the words to express yourself,” Guerrero told the Daily Herald of Illinois for a report on language barriers to mental health care. “It’s not the feeling itself, but the ability to communicate what you are experiencing.”
The consequences of poor communication are grim.
People may not get the treatment they need, and get worse and worse, Majose Carrasco of the National Latino Behavioral Health Association, told Pew Charitable Trusts.
“You could have suicide. You could have people ending up homeless or in jail,” she said.
Latinos and Mental Health
Nearly 1 in 5 Latinos suffers a mental health problem.
But Latinos are less likely than other groups to seek out treatment for mental health conditions, such as depression, anxiety, stress, etc.
They fear being stigmatized. They lack of health insurance. They face cultural barriers. Or they simply a fail to recognize symptoms, Salud America! reported in April 2017.
“It’s difficult to trust that translation will capture nuances in the soul-baring process of mental health treatment,” Sita Diehl of the National Alliance on Mental Illness, told Pew in 2015.
Mental Health Professional Shortage
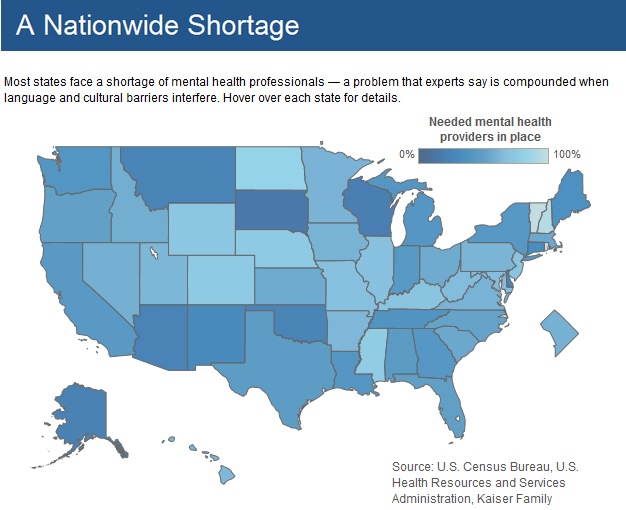 The biggest shortages of mental health professionals were in South Dakota, Wisconsin, Alaska, Arizona and Oklahoma, Pew Charitable Trusts reports.
The biggest shortages of mental health professionals were in South Dakota, Wisconsin, Alaska, Arizona and Oklahoma, Pew Charitable Trusts reports.
These areas have only a quarter or less of needed psychiatrists, counselors and therapists.
“Culture and language barriers have complicated the issue in places like Alaska, which saw a string of suicides this fall among Alaska Natives, and New Mexico and Arizona, which have large numbers of Spanish and Navajo speakers,” according to the report.
And this gap is only going to grow.
The nation needs to add 10,000 providers to each of seven separate mental healthcare professions by 2025 to meet the expected growth in demand, Modern Healthcare reports.
Potential Solutions
Several solutions exist to fix the shortage of mental health professionals.
Integrating behavioral health services within primary care settings is one key.
“Mental health screenings during a primary care visit can identify patients suffering from stress, anxiety and depression. Quick referrals and appointments with specialists can prevent more severe health issues down the road,” according to Modern Healthcare.
 Telemental health is another emerging solution.
Telemental health is another emerging solution.
In April 2017, the American Telemedicine Association issued new guidelines that allow for treatment of mental and behavioral health services to children and adolescents using videoconferencing, we reported in May 2017.
More training of health professionals also is needed.
Some organizations in Texas give scholarships to bilingual mental health students.
Dr. Irán Barrera’s Consejo project at Fresno State trains social work students to deliver mental health services and other support to Spanish-speaking children, teens, and families in the San Joaquin Valley, we reported in March 2017.
The Consejo project has two goals.
First is to examine and eliminate the mental health care barriers in the area. Second is to increase the number of local bilingual behavioral health professionals.
The California Social Work Education Center at the University of California, Berkeley, has a contract with the state to encourage more diverse and bilingual students to study mental health as part of graduate studies in social work, Pew Charitable Trusts reports.
Also in California and New Mexico, officials are working to identify homegrown candidates from needy communities, and helping them to pay for education in the field or to pay off student loans if they return home to work in mental health fields, Pew also reported.
“We need to give students the opportunity to get exposed and decide for themselves,” Carrasco told Pew. “We tell them, ‘You can come back and help your community.’ To them this is very empowering.”
By The Numbers
142
Percent
Expected rise in Latino cancer cases in coming years



