
Share On Social!
Most Americans living in rural communities say they are content with most aspects of their lives; however, two significant concerns stand out: Financial insecurity and the high medical costs.
Two surveys, conducted through a partnership between NPR, Robert Wood Johnson Foundation, and the Harvard T.H. Chan School of Public Health, found that 40% of that demographic struggle with healthcare, housing, and food expenses.
Healthcare Access, or Lack There Of
The surveys also found that 26% of rural Americans said they had not received desperately needed medical attention due to their limited budget. However, nine in 10 respondents did report having health insurance. An increase that is attributed to the implementation Affordable Care Act and Medicaid expansion.
A decade ago, this was not the case.
“At a time when we thought we had made major progress in reducing barriers to needed health care, the fact that one in four still face these barriers is an issue of national concern,” said Robert J. Blendon, co-director of the survey and professor of health policy and political analysis at the Harvard T.H. Chan School of Public Health.
“Either it is still not affordable for them, or the insurance they have doesn’t work — or they can’t get care from the health providers that are in their community.”
Financial Insecurities’ Role
When it comes to economic stability, rural Americans fare poorly.
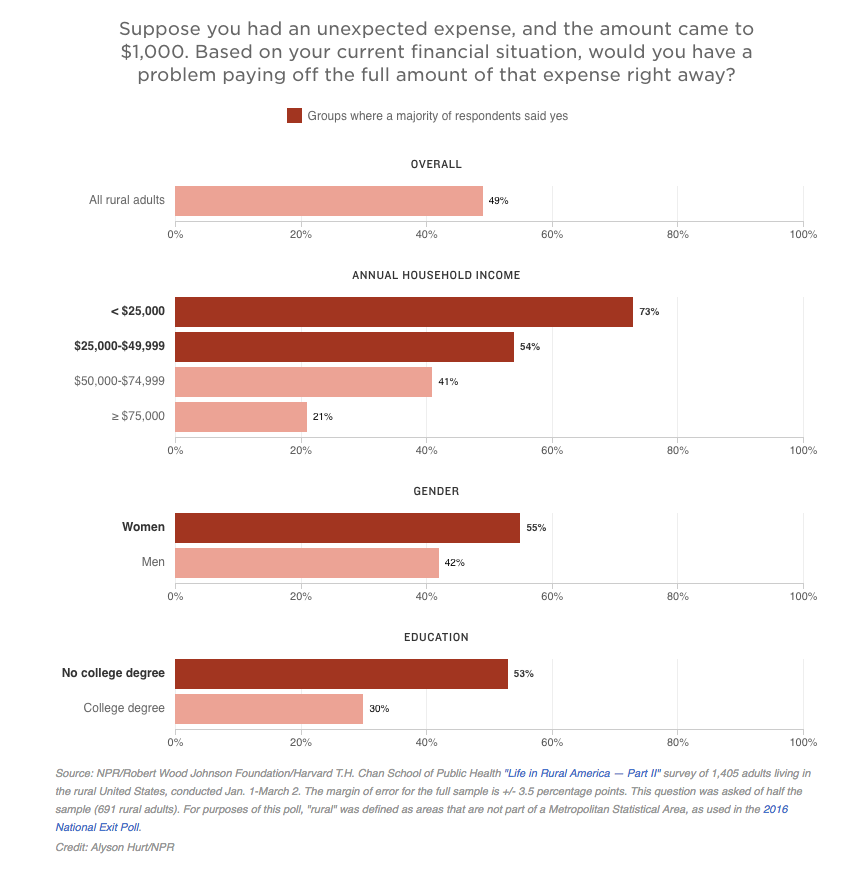
Nearly half (49%) of the respondents said they could not afford to pay an unexpected $1,000 expense of any type.
It’s even worse for minority communities.
A significant 62% of rural Latinos said it would be challenging to pay a $1,000 expense, compared to 45% of rural whites.
Moreover, 68% of rural Blacks experience similar insecurities.
“When you’re living close to the edge, sometimes you fall off,” said Dee Davis, president and founder of the Center for Rural Strategies. “If half the people in rural America can’t deal with a $1,000 bill, that’s rough.”
Medical Deserts Rural America
Hospital Deserts
Since 2010, 5% of rural hospitals have closed their doors. Worse, maternal and obstetric caretaking has taken the hardest hit.
This problem is not improving either. Currently, 673 rural hospitals are at risk of being closed.
There is a need, however, for vital medical attention in these communities. Accidental deaths occur at a 50% higher rate in rural areas when compared to urban areas.
“It means people have to travel greater distances to receive care, and distance can be a barrier to timely and appropriate access to services,” Brock Slabach of the National Rural Health Assembly said.
“Delayed care can often lead to tragic consequences. This can be a huge barrier for many living in rural areas.”
Pharmacy Deserts
Hospitals are not the only healthcare facilities closing. Pharmacies are on the same path.
In the last 16 years, 1,231 rural, independently-owned pharmacies have closed. That’s 16% of all drugstores in those towns.
Unfortunately, fewer than 6,400 pharmacies are left in these communities.
Childcare Deserts
Childcare deserts adversely affect Latinos and rural communities.
60% of Latinos live in regions that have a shortage of licensed child care centers.
Furthermore, nearly 60% of rural communities are in the same situation.
Davis made one thing clear: his neighbors in Whitesburg, Kentucky (1.97% Latino) are experiencing a crisis of financial insecurity and lack of healthcare.
“People in this congressional district have the shortest life span in the United States; we also are the poorest,” Davis said. “We’re poor, and we’re sicker.”
Explore More:
AccessBy The Numbers
25.1
percent
of Latinos remain without health insurance coverage



