Share On Social!
Chronic liver disease can wreak havoc on the body, especially when there is a viral illness spreading worldwide.
People suffering from Non-alcoholic Fatty Liver Disease (NAFLD) are roughly three times as likely to die from coronavirus than those who did not suffer from any liver disease, according to a recent study done at Sheba Medical Center.
“It’s possible that the coronavirus damages the liver similarly to the way in which it attacks the lungs,” Professor Ziv Ben Ari, head of the Center for Liver Diseases at Sheba Medical Center, told The Jerusalem Post. “It is also possible that the damage to the liver is done by the medicine given to the patient to treat COVID-19 or an immunological reaction caused by the virus, which causes a Cytokine storm, which causes a liver infection.”
New Studies about Chronic Liver Disease and COVID-19
Chronic liver disease (CLD) and liver cancer are major public health concerns, especially worldwide.
This is not good news for people of color, who are disproportionately affected by liver disease amid a pandemic that is worsening historical inequities.
Over the past two decades, Latinos, in particular, have suffered a rise in CLD prevalence. More than that, they are experiencing high rates of COVID-19 cases and deaths.
Worse, cancer patients who get COVID-19 have a higher risk of dying from the illness. Much higher—13% higher, in fact—than the death rate of coronavirus in the general population, which is at about 6%.
Hepatocellular carcinoma (HCC), representing 78% of all liver cancers, is highly fatal, with only 18% of patients surviving 5 years in the U.S.
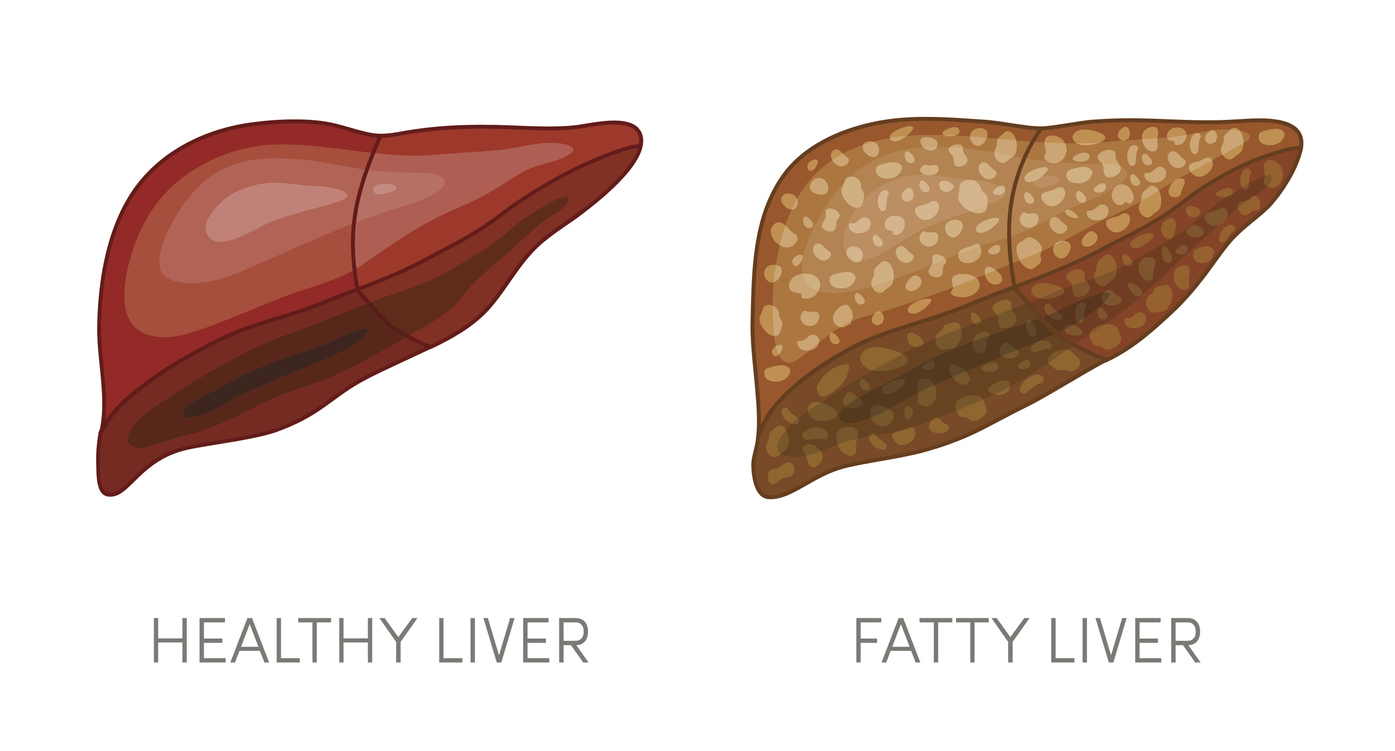
With the rapid spread of the COVID-19 pandemic, health experts have expressed significant concern that Latino patients with CLD and HCC are at higher risk for complications.
People suffering from liver diseases are more at risk from COVID-19, many recent studies published in the Journal of Hepatology and other reputed journals suggested.
In another study, the Yale Liver Center researchers found that patients with COVID-19 presented with abnormal liver tests at much higher rates.
The data suggest that higher levels of liver enzymes, mainly proteins released when the liver is damaged, were associated with poorer outcomes for these patients, including ICU admission, mechanical ventilation, and death.
“Liver disease is widespread in the U.S. population,” Dr. Michael Nathanson, the Yale Liver Center director, and a co-author of the study, told the Yale News. “In the U.S., close to one-third of people have fatty liver disease, and several million people have chronic hepatitis B or C.”
Many researchers believe that most COVID-19-induced liver-mortality will be delayed, mainly from deferred care for liver diseases, reduced funding for public health interventions, and the global economic crisis.
All this could lead to increases in alcohol and drug use and in blood-borne virus transmissions while access to care and funding is reduced.
Why Are these Liver Disease Studies Important for Latinos?
The coronavirus can affect anyone. But many studies and reports show that Latinos and other people of color are disproportionately affected.
“Obesity and metabolic syndrome-related disease are growing concern in Latino community,” said Dr. Rita Lepe, director of hepatology health care disparities at Texas Liver Institute in Dallas.
Lepe is fluent in Spanish, born and raised in Mexico, actively volunteers in community service, and does medical missionary work in Latin America and the Mexican consulate.

“A lack of access to healthy, language barrier, lack of access to the information and sustainable food is causing Latinos to develop severe liver diseases and related health problems at young age,” Lepe said.
“Often Latino kids with childhood obesity develop chronic medical problems and having early onset of diabetics, which leads to kidney transplantation in their teens and liver disease in their 40s,” Lepe said.
In adults, 1 in 4 Americans will fight liver disease, called NASH (nonalcoholic steatohepatitis). For Latino adults, specifically those of Mexican and Central American descent, that rate is drastically higher.
About 1 in 3 middle-aged Latinos in South Texas have NASH.
Studies show that NASH-associated HCC is the third-most-common cause of HCC in the US. NASH is an asymptomatic “silent” disease. Most patients show no symptoms, and most people with NASH are not diagnosed.
“The increased rate and severity of NASH in Latino Americans likely is related to the interplay between issues such as genetic factors, access to health care, or the prevalence of chronic diseases such as metabolic syndrome or diabetes.
What Efforts Aim to Reduce Fatty Liver Disease?
“A lot of work and support is needed to change the current situation,” Lepe said.

On NASH Day on June 12, the expert manifesto was published, and events took place around the world to raise awareness and inspire action.
“Many people are unaware of the severity of NASH and fatty liver, and in mainly Latino patients, it is detected very late, which results in missing many opportunities to treat and prevent the outcome,” Lepe said
To learn more about NASH and non-alcoholic liver disease, visit the NIH website.
Amid the COVID-19 pandemic, it is important to follow the CDC guidelines. The CDC has compiled tips on what people can do to help slow the spread of the new coronavirus and make homes, schools, and workplaces safer. This includes not shaking hands and avoiding large crowds and non-essential travel.
Share our Salud America! “Juntos, We Can Stop COVID-19” digital communication campaign in English or Spanish to help Latino families and workers take action to slow the spread of coronavirus, including getting the vaccine when available.
The #JuntosStopCovid campaign features culturally relevant fact sheets, infographics, and video role model stories to encourage Latinos to practice safe public health behaviors.
Also, learn more about the coronavirus pandemic and its implications concerning Latino health.
By The Numbers
142
Percent
Expected rise in Latino cancer cases in coming years



